WUNRN
http://www.thelancet.com/journals/langlo/article/PIIS2214-109X%2814%2970219-0/fulltext
The Lancet Global Health, Volume 2, Issue 6, Pages e311 - e312, June 2014
HIV/AIDS - Tackling Stigma: Fundamental to an AIDS-Free Future – Women
& Girls
Julie Pulerwitz a, John Bongaarts b
The achievement of an
AIDS-free future will surely be a priority discussion topic at the upcoming
International AIDS Society conference in Melbourne, Australia. The discovery
that antiretroviral therapy (ART) limits HIV transmission1 follows
several years of steady progress in controlling the epidemic, with the number
of new HIV infections falling from 3·7 million in 1997 to 2·3 million, and AIDS
deaths from 2·3 million in 2005 to 1·6 million in 2012.2 Nevertheless,
the number of people living with HIV is still rising as the number of new
infections exceeds the number of deaths in this group. Moreover, coverage of
ART in people meeting even the 2010 WHO standard for treatment (ie, CD4 cell
count <350 cells/μL) is still far from complete, and plans to expand
treatment to cover all people living with HIV for the rest of their lives are
viewed with scepticism by some people.3 Crucial
international funding for HIV and AIDS has remained static for several years.2 Although
funding from national budgets is rising, countries will find it very difficult
to cover the growing cost of treatment, especially when the more expansive 2013
WHO standard (ie, CD4 cell count <500 cells/μL) is applied.
Sub-Saharan Africa remains
the region most affected by HIV, but the rapid scale-up of ART programmes has
had clear results: the number of AIDS deaths—which has risen steadily since the
1970s and peaked in 2004—05 at 1·8 million—fell to 1·2 million by 2012.4 In the
African region, an equally important but underappreciated reason for the recent
decline in deaths is the peaking of new infections in 1997 at 2·7 million. Most
of the subsequent decrease to 1·6 million new infections in 2012 occurred
before ART became widely available in the mid-2000s. Instead, behavioural
change in response to the threat of AIDS and to prevention efforts underlies
this trend. Its effect is well documented in Uganda and Zimbabwe,5, 6 but reductions in risky
behaviour have also occurred in other countries.2 One of the
most striking trends since the early 1990s7 is the rise
in condom use in women not in marital unions (figure). This trend seems to be
an important reason why infection rates in young women have fallen sharply.
Without the change in behaviour and resulting decline in HIV incidence, the
number of AIDS-related deaths in sub-Saharan Africa would now be substantially
higher than it actually is.
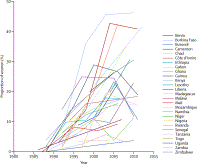
Condom
use in women not in marital union in Africa
Data
are from DHSSTATcompiler.7
However, millions of
people are still becoming infected with HIV every year, and key populations
such as sex workers, injection drug users, and men who have sex with men are
disproportionately affected. Compared with the general population, men who have
sex with men and sex workers are 13·5 times more likely to be infected with
HIV, and injection drug users are 20 times more likely to be infected with the
virus.8 Although the
overall prevalence of HIV is falling, epidemics in these key groups are
expanding in many places worldwide.9 Prevention of
HIV in these marginalised groups is difficult to address because of stigma,
discrimination, and their sequelae.2, 10, 11 Key populations actually
experience a double stigma related to both being associated with HIV and the
reinforcement of pre-existing stigmas.12 This
situation has led to inadequate access to service provision and treatment, in
addition to many other negative outcomes. Increasing evidence indicates that
“prevention basics for key populations can be highly effective”.13 Calls are
growing to bring behavioural approaches, including harm reduction and condom
promotion, “back to the centre of the debate for HIV prevention”.14, 15 To more effectively reach
key populations with the prevention basics, explicit reduction in HIV stigma
should be made a priority. One notable example is HIV counselling and testing,
a health system entry point that can address both prevention or treatment and
care objectives, including treatment as prevention. Stigma inhibits the use of
HIV counselling and testing, and evidence suggests that addressing of stigma
will probably increase access to and use of HIV counselling and testing.16
Stigma and discrimination
experienced by sex workers, injection drug users, and men who have sex with men
is tough to tackle. Responses need to be tailored to very different
circumstances and require interventions on several levels: policy, societal,
health system, and individual. There is no magic bullet response, however, many
examples exist of stigma-reduction strategies and programmes with proven
effectiveness.17—19 The effects of such
programmes have often been limited because they are rarely taken to scale, and
appropriate targeting to and tailoring for key populations has not been done
frequently.
Funding to address stigma
confronts two problems: not only do general primary prevention strategies (such
as the promotion of behaviour change) suffer from “striking underfunding”3 but also
prevention efforts for key populations remain minimum to non-existent
throughout much of the world.2 Additionally,
90% of current HIV programme funds for sex workers, injection drug users, and
men who have sex with men come from international donors.8 Without more
political and economic commitment from local governments, the needs of key
populations will be difficult to address.
It is hard to envision
that significant progress will continue to be made in HIV prevention efforts
with key populations without a prioritisation of stigma reduction and the
allocation of adequate funding for behavioural and social change. The
importance of tackling stigma has long been recognised, and now is the time to
put stigma reduction at the forefront of programmatic responses.
We declare no competing
interests.
References
1 Cohen M, Chen Y, McCauley M, et al.
Prevention of HIV-1 infection with early antiretroviral therapy. N Engl J
Med 2011; 365: 493-505. CrossRef | PubMed
2 UNAIDS. Global report: UNAIDS report on the
global AIDS epidemic 2013. http://www.unaids.org/en/media/unaids/contentassets/documents/epidemiology/2013/gr2013/UNAIDS_Global_Report_2013_en.pdf.
(accessed Feb 12, 2014)
3 Shelton J. HIV/AIDS. ARVs as prevention: a
tough road to wide impact. Science 2011; 334: 1645-1646. CrossRef | PubMed
4 UNAIDS. AIDSINFO website. http://www.unaids.org/en/dataanalysis/datatools/aidsinfo/.
(accessed Jan 22, 2014).
5 Stoneburner RL, Low-Beer D. Population-level
HIV declines and behavioral risk avoidance in Uganda. Science 2004; 304:
714-718. CrossRef | PubMed
6 Gregson S, Garnett G, Nyamukapa C, et al.
HIV decline associated with behavior change in eastern Zimbabwe. Science
2006; 311: 664-666. CrossRef | PubMed
7 USAID. STATcompiler. http://www.statcompiler.com/.
(accessed Jan 22, 2014).
8 UNAIDS. Global report: UNAIDS report on the
global AIDS epidemic 2012. http://www.unaids.org/en/media/unaids/contentassets/documents/epidemiology/2012/gr2012/20121120_UNAIDS_Global_Report_2012_with_annexes_en.pdf.
(accessed Feb 12, 2014).
9 Beyrer C, Baral S, van Griensven F, et al.
Global epidemiology of HIV infection in men who have sex with men. Lancet
2012; 380: 367-377. Summary | Full Text | PDF(757KB) | CrossRef | PubMed
10 Altman D, Aggleton P, Williams M, et al.
Men who have sex with men: stigma and discrimination. Lancet 2012; 380:
439-445. Full Text | PDF(88KB) | CrossRef | PubMed
11 Beyrer C, Malinowska-Sempruch K,
Kamarulzaman A, et al. 12 myths about HIV/AIDS and people who use drugs. Lancet
2010; 376: 208-211. Full Text | PDF(326KB) | CrossRef | PubMed
12 Parker R, Aggleton P. HIV and AIDS-related
stigma and discrimination: a conceptual framework and implications for action. Soc
Sci Med 2003; 57: 13-24. CrossRef | PubMed
13 Laga M. Effect of HIV prevention in key
populations: evidence accumulates, time to implement. Lancet Glob Health
2013; 1: e243-e244. PubMed
14 Laga M, Piot P. Prevention of sexual
transmission of HIV: real results, science progressing, societies remaining
behind. AIDS 2012; 26: 1223-1229. CrossRef | PubMed
15 Beyrer C, Malinowska-Sempruch K,
Kamarulzaman A, Kazatchkine M, Sidibe M, Strathdee S. Time to act: a call for
comprehensive responses in HIV in people who use drugs. Lancet 2010; 376:
551-563. Summary | Full Text | PDF(647KB) | CrossRef | PubMed
16 Obermeyer CM, Osborn M. The utilization of
testing and counseling for HIV: a review of the social and behavioral evidence.
Am J Public Health 2007; 97: 1762-1774. CrossRef | PubMed
17 Mahajan AP, Sayles JN, Patel VA, et al.
Stigma in the HIV/AIDS epidemic: a review of the literature and recommendations
for the way forward. AIDS 2008; 22: S67-S79. CrossRef | PubMed
18 Pulerwitz J, Michaelis A, Weiss E, Brown L,
Mahendra V. Reducing HIV-related stigma: lessons learned from Horizons research
and programs. Public Health Rep 2010; 125: 272-281. PubMed
19 Sengupta S, Banks B, Jonas D, Miles MS,
Smith GC. HIV interventions to reduce HIV/AIDS stigma: a systematic review. AIDS
Behav 2011; 15: 1075-1087. CrossRef | PubMed