WUNRN
Posted by WUNRN for women’s and girls’ right to food, food security, nutrition, health, and quality of life.
McKinsey Global Institute
GO TO WEBSITE LINK ABOVE TO CLICK TO FULL REPORT & EXECUTIVE SUMMARY.
How the World Could Better Fight
Obesity
November 2014 | By Richard Dobbs, Corinne Sawers, Fraser Thompson, James Manyika, Jonathan Woetzel, Peter Child, Sorcha McKenna, and Angela Spatharou
Box 1. The complex causes of obesity
The root causes of rising
obesity are highly complex, spanning evolutionary, biological, psychological,
sociological,
economic, and institutional
factors. The UK government Foresight research on obesity identified more than
100
variables that directly or
indirectly affect obesity outcomes (Exhibit 1).
Because of centuries of food
insecurity, human beings have evolved with a biological ability to cope with
food scarcity rather
than abundance. The human body
seeks out energy-dense foods and tries to conserve energy as fat. Hormones that
regulate
hunger and satiety encourage
people to seek extra food when food is scarce but do not seem to have the
ability to prevent
over-consumption or encourage
extra calorie burning when food is abundant. Modern life makes fewer physical
demands on many
people, who lead less active
lifestyles as technology replaces the need for physical labor. With many jobs
now sedentary, exercise
is a conscious and optional
choice.
As an illustration of the
change, in 1969 about 40 percent of US schoolchildren walked or rode their
bikes to school; by 2001, only
13 percent did.1 Over the past 50 years, it has been estimated that a reduction in
occupation-related physical
activity in the United States has reduced the daily net energy balance by 100
calories
per person, a significant share
of the overall change in the energy balance during this period.2
Mass urbanization in many
regions—the global urban population is growing by 65 million a year, the
equivalent of
adding seven new cities the size
of Chicago every 12 months—is boosting incomes but reinforcing a less physical
lifestyle.3 One
Chinese study found that urbanization reduces daily energy expenditure by 300
to 400 calories, and
traveling to work by car or bus
reduces it by a further 200 calories.4
Human beings also have a
psychological relationship with food that goes beyond a need for basic
sustenance.
Many of us use food as a reward
or to relieve stress, or have a compulsive relationship with certain types of
food.
There is a correlation between
obesity and high rates of some mental health conditions, including depression.
1 Noreen C. McDonald, “Active
transportation to school: Trends among US schoolchildren, 1969–2001,” American
Journal of
Preventative Medicine, volume
32, issue 6, June 2007.
2 T. S. Church et al., “Trends
over 5 decades in US occupation-related physical activity and their
associations with obesity,” PLoS ONE,
volume 6, number 5, 2011.
3 For more on urbanization, see,
for example, Urban world: Mapping the economic power of cities,
McKinsey Global Institute,
March 2011.
4 W. P. James, “The fundamental
drivers of the obesity epidemic,” Obesity Reviews, volume
9, supplement 1, March 2008.
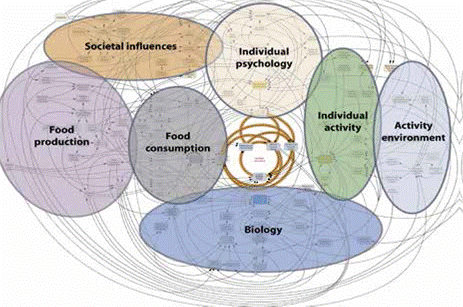
Academics have emphasized that obesity
is a systemic problem:
causes are complex, manifold, and
interdependent
Obesity causal map
SOURCE: B. Butland et al., Foresight:
Tackling obesities—future choices, UK Government Office for Science, project
report, 2nd ed., October 2007.
Exhibit 1
Media Social Psychological Economic Food
Activity Infrastructure Developmental
Biological Medical
Positive influence
Negative influence
Overcoming obesity: An initial
economic analysis 13
McKinsey Global Institute
Box 1. The complex causes of obesity
(continued)
People are highly influenced by
social norms and subtle social cues in their eating habits and their attitude
toward
weight. For instance, if they
dine with other people who eat more, they eat more themselves; likewise, those
who
dine with people who eat less,
eat less themselves. One study has shown that 35 percent more calories are
consumed when having dinner with
a friend than when eating alone, and 96 percent more if dining in a group of
seven people.5 Another
study has shown that a person is 57 percent more likely to become obese if a
friend has
also become obese—evidence of
social normalization of the condition.6
Food has become much more
affordable over the past 60 years. In the United States, the share of average
household income spent on food
fell from 42 percent in 1900 to 30 percent in 1950 and to 13.5 percent in 2003.7
This is beneficial in welfare
terms, reducing rates of undernutrition and freeing up disposable income.
Many of these factors underline
the importance of the environmental context as a driver of obesity prevalence.
A helpful lens for examining how
the environment affects prevalence is looking at expatriate populations,
transplanted from one context to
another. For example, British expats who have settled in Abu Dhabi have
diabetes prevalence rates of 18
percent, compared with a baseline prevalence of 8 percent in the United
Kingdom.
Physical environment is one
factor, but it is likely that sociocultural variables are also relevant.
Various studies
suggest a correlation between
Hispanic immigrants’ obesity rate and the length of their stay in the United
States
and the depth of their cultural
assimilation.8
Some experts are questioning
whether the net energy balance—that people are eating too much and exercising
too little—is the appropriate
lens to examine root causes. There is growing interest in the role that
different
nutrients such as carbohydrates,
proteins, and fats play in our metabolism and in hormones that regulate satiety
and hunger. Many leading
scientists support the view that refined carbohydrates promote weight gain and
inhibit
weight loss.9 The
science to date on this is inconclusive, and we do not include it in the
assessment here without
further evidence. However, it is
an important area for further research and could refocus the design of obesity
interventions. Similarly, there
is increasing interest in the role of the microbiome—our intestinal bacteria
ecosystem.
Scientific evidence from
controlled trials suggests that individuals whose bodies contain a greater
diversity of
bacterial species are less prone
to high body mass index (BMI) and less likely to gain weight.10 This also
is too
inconclusive for us to include
at this stage.
Some commentators take the
causal complexity illustrated in Exhibit 1 as a pre-determined defeat. They
say, “If
the causes are so complex, where
do we begin?” However, we do have a good understanding of the proximate
causes, even if the background
causes are complex. We know that over the past 50 years, individuals’ daily
energy balance equation has
changed; physical activity has declined, and energy consumption has increased.
Even though there are important
outstanding questions about diet composition, gut microbiome, and epigenetics,
we are not walking blind with no
sense of what to address. However,
interventions to increase physical activity,
reduce energy consumption, and address diet
composition cannot just seek to reverse the historical trends that
have left the population where it is today.
For example, we cannot, nor would we wish to, reverse the invention
of the Internet or the industrialization of
agriculture. We need to assess what interventions make sense and are
feasible in 2014.
5 Brian Wansink, Mindless eating:
Why we eat more than we think, Bantam-Dell, 2006.
6 Nicholas A. Christakis and James H.
Fowler, “The spread of obesity in a large social network over 32 years,” New England Journal
of
Medicine, volume 357, number 4, July 2007.
7 100 years of US consumer spending data for
the nation, New York City, and Boston, US Department of Labor, report number 991,
May 2006.
8 D. A. Himmelgreen et al., “The longer you
stay, the bigger you get: Length of time in the US and language are associated
with obesity
in Puerto Rican women,” American Journal of
Physical Anthropology,
volume 125, number 1, 2004.
9 B. J. Brehm et al., “The role of energy
expenditure in the differential weight loss in obese women on low-fat and
low-carbohydrate
diets,” Journal of Clinical Endocrinology
and Metabolism,
volume 90, number 3, March 2005.
10 Herbert Tilg and Arthur Kaser, “Gut
microbiome, obesity and metabolic dysfunction,” Journal of Clinical
Investigation,
volume 121,
number 6, June 2011.