WUNRN
MAMMOGRAMS - VAST STUDY RAISES
QUESTIONS FOR FURTHER REVIEW
Direct Link to Research Report - 25
Years, 90,000 Women:
One of the largest and most meticulous studies of mammography ever done,
involving 90,000 women and lasting a quarter-century, has added powerful new
doubts about the value of the screening test for women of any age.
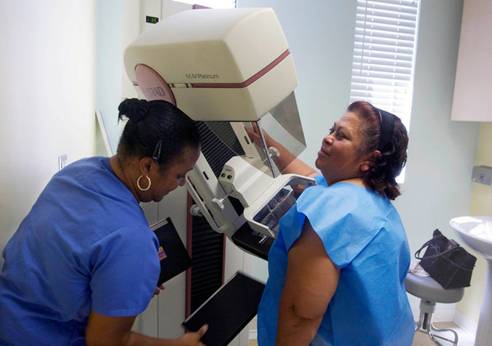
Nearly 75 percent of American women 40 and over
say they had a mammogram in the past year. Damian
Dovarganes/Associated Press
It found that the death rates from breast
cancer and from all causes were the same in women who got mammograms and those
who did not. And the screening had harms: One in five cancers found with
mammography and treated was not a threat to the woman’s health and did not need
treatment such as chemotherapy, surgery or radiation.
The study,
published Tuesday in The British Medical Journal, is one of the few rigorous
evaluations of mammograms conducted in the modern era of more effective breast
cancer treatments. It randomly assigned Canadian women to have regular
mammograms and breast exams by trained nurses or to have breast exams alone.
Study
Results
A large, 25-year study of Canadian women aged 40 to 59 found no benefit for women who were randomly assigned to have mammograms.
The death rate
from breast cancer was the same in both groups, but 1 in 424 women who
had mammograms received unnecessary cancer treatment, including surgery,
chemotheraphy and radiation.
British Medical Journal
The study seems likely to lead to
an even deeper polarization between those who believe that regular mammography
saves lives, including many breast cancer patients and advocates for them, and
a growing number of researchers who say the evidence is lacking or, at the very
least, murky.
“It will make women uncomfortable, and
they should be uncomfortable,” said Dr. Russell P. Harris, a screening expert
and professor of medicine at the
The findings will not lead to any
immediate change in guidelines for mammography, and many advocates and experts
will almost certainly dispute the idea that mammograms are on balance useless,
or even harmful.
Dr. Richard C. Wender, chief of cancer
control for the American Cancer Society, said the society had convened an
expert panel that was reviewing all studies on mammography, including the
Canadian one, and would issue revised guidelines later this year. He added that
combined data from clinical trials of mammography showed it reduces the death
rate from breast cancer by at least 15 percent for women in their 40s and by at
least 20 percent for older women.
That means that one woman in 1,000 who
starts screening in her 40s, two who start in their 50s and three who start in
their 60s will avoid a breast cancer death, Dr. Harris said.
Dr.
Wender added that while improved treatments clearly helped lower the breast
cancer death rate, so did mammography, by catching cancers early.
But an editorial accompanying the new study
said that earlier studies that found mammograms helped women were done before
the routine use of drugs like tamoxifen
that sharply reduced the breast cancer death rate. In addition, many studies
did not use the gold-standard methods of the clinical trial, randomly assigning
women to be screened or not, noted the editorial’s author, Dr. Mette Kalager,
and other experts.
Dr. Kalager, an epidemiologist and
screening researcher at the
“It might be possible that mammography
screening would work if you don’t have any awareness of the disease,” she said.
The Canadian study reached the same
conclusion about the lack of a benefit from mammograms after 11 to 16 years of
follow-up, but some experts predicted that as time went on the advantages would
emerge.
That did not happen, but with more time the researchers could, for the
first time, calculate the extent of overdiagnosis, finding cancers that would
never have killed the women but that led to treatments that included surgery,
chemotherapy and radiation.
Many
cancers, researchers now recognize, grow slowly, or not at all, and do not
require treatment. Some cancers even shrink or disappear on their own. But once
cancer is detected, it is impossible to know if it is dangerous, so doctors
treat them all.
Mammography’s benefits have long been
debated, but no nations except
Dr. Peter Juni, a member of the Swiss
Medical Board until recently, said one concern was that mammography was not reducing
the overall death rate from the disease, but increasing overdiagnosis and
leading to false positives and needless biopsies.
“The mammography story is just not such an
easy story,” said Dr. Juni, a clinical epidemiologist at the
Even experts like Dr. H. Gilbert Welch, a
professor of medicine at
In the
Dr. Kalager, whose editorial accompanying
the study was titled “Too Much Mammography,” compared mammography to prostate-specific
antigen screening for prostate cancer, using data from pooled
analyses of clinical trials. It turned out that the two screening tests were
almost identical in their overdiagnosis rate and had almost the same slight
reduction in breast or prostate deaths.
“I was very surprised,” Dr. Kalager said.
She had assumed that the evidence for mammography must be stronger since most
countries support mammography screening and most discourage PSA screening.