WUNRN
What is chlamydia?
Chlamydia
is a common sexually transmitted disease (STD) caused by a bacterium. Chlamydia
can infect both men and women and can cause serious, permanent damage to a
woman's reproductive organs.
How common is chlamydia?
Chlamydia is the most frequently
reported bacterial sexually transmitted infection in the
How do people get chlamydia?
People get chlamydia by having
sex with someone who has the infection. “Having sex” means anal, vaginal, or
oral sex. Chlamydia can still be transmitted even if a man does not ejaculate.
People who have had chlamydia and have been treated can get infected again if they
have sex with an infected person.
Chlamydia can also be spread from an infected
woman to her baby during childbirth.
Who is at risk for chlamydia?
Any sexually active person can be
infected with chlamydia. It is a very common STD, especially among young
people. It is estimated that 1 in 15 sexually active females aged 14-19
years has chlamydia.
Sexually active young people are
at high risk of acquiring chlamydia for a combination of behavioral and
biological reasons. Men who have sex with men (MSM) are also at risk for
chlamydial infection since chlamydia can be transmitted by oral or anal sex.
What are the symptoms of chlamydia?
Chlamydia is known as a ‘silent’ infection
because most infected people have no symptoms. If symptoms do occur, they may
not appear until several weeks after exposure. Even when it causes no symptoms,
chlamydia can damage a woman’s reproductive organs.
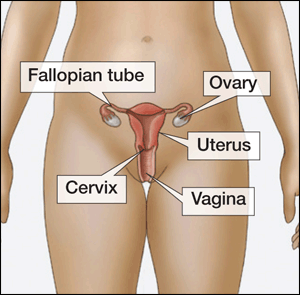
In women, the bacteria first
infect the cervix (structure that connects the vagina or birth canal to the
uterus or womb) and/or the urethra (urine canal). Some infected women have an
abnormal vaginal discharge or a burning sensation when urinating. Untreated
infections can spread upward to the uterus and fallopian tubes (tubes that
carry fertilized eggs from the ovaries to the uterus), causing pelvic
inflammatory disease (PID). PID can be silent, or can cause symptoms such as
abdominal and pelvic pain. Even if PID causes no symptoms initially, it can
lead to infertility (not being able to get pregnant) and other complications
later on.
Some infected men have discharge
from their penis or a burning sensation when urinating. Pain and swelling in
one or both testicles (known as “epididymitis”) may also occur, but is less
common.
Chlamydia can also infect the
rectum in men and women, either through receptive anal sex, or possibly via
spread from the cervix and vagina. While these infections often cause no
symptoms, they can cause rectal pain, discharge, and/or bleeding (known as
“proctitis”).
What complications can result from
chlamydial infection?
The initial damage that chlamydia
causes often goes unnoticed. However, chlamydial infections can lead to serious
health problems.
In women, untreated infection can
spread upward to the uterus and fallopian tubes (tubes that carry fertilized eggs
from the ovaries to the uterus), causing pelvic
inflammatory disease (PID). PID can be silent, or can cause
symptoms such as abdominal and pelvic pain. Both symptomatic and silent PID can
cause permanent damage to a woman’s reproductive tract and lead to long-term
pelvic pain, inability to get
pregnant, and potentially deadly
ectopic pregnancy (pregnancy outside the uterus).
In pregnant women, untreated
chlamydia has been associated with pre-term delivery, and can spread to the
newborn, causing an eye infection or pneumonia.
Complications are rare in men.
Infection sometimes spreads to the tube that carries sperm from the testis,
causing pain, fever, and, rarely, preventing a man from being able to father
children.
What about chlamydia and HIV?
Untreated chlamydia may increase
a person’s chances of acquiring or transmitting HIV – the virus that causes
AIDS.
How does chlamydia affect a pregnant
woman and her baby?
In pregnant women,
untreated chlamydia has been associated with pre-term delivery, and can spread
to the newborn, causing an eye infection or pneumonia. Screening and treatment
of chlamydia during pregnancy is the best way to prevent these complications.
All pregnant women should be screened for chlamydia at their first prenatal
visit.
Who should be tested for chlamydia?
Any sexually active person can be
infected with chlamydia. Anyone with genital symptoms such as discharge,
burning during urination, unusual sores, or rash should avoid having sex until
they are able to see a health care provider about their symptoms.
Also, anyone with an oral, anal,
or vaginal sex partner who has been recently diagnosed with an STD should see a
health care provider for evaluation.
CDC recommends yearly chlamydia
testing for all sexually active women age 25 or younger and older women with
risk factors for chlamydial infections (e.g., women who have a new or more than
one sex partner), and all pregnant women. Any woman who is sexually active
should discuss her risk factors with a health care provider who can then
determine if more frequent testing is necessary.
Men who have sex with men (MSM)
who have receptive anal sex should be tested for chlamydia each year. MSM who
have multiple and/or anonymous sex partners should be tested more frequently.
HIV-infected sexually active
women who are age 25 or younger or have other risk factors, and all
HIV-infected patients who report having receptive anal sex should be tested for
chlamydia at their first HIV care visit and then at least annually. A patient’s
health care provider might determine more frequent testing is necessary, based
on the patient’s risk factors.
How is chlamydia diagnosed?
There are laboratory tests to
diagnose chlamydia. Specimens commonly used for testing include a cotton swab
of the vagina (collected by the woman herself or her health care provider) or a
urine sample.
What is the treatment for chlamydia?
Chlamydia can be easily treated
and cured with antibiotics. HIV-positive persons with chlamydia should receive
the same treatment as those who are HIV-negative.
Persons with chlamydia should
abstain from having sex for seven days after single dose antibiotics, or until
completion of a seven-day course of antibiotics, to prevent spreading the
infection to partners.
Repeat infection with chlamydia
is common. Persons whose sex partners have not been appropriately treated are
at high risk for re-infection. Having multiple chlamydial infections increases
a woman's risk of serious reproductive health complications, including pelvic
inflammatory disease and ectopic pregnancy. Women and men with chlamydia
should be retested about three months after treatment of an initial infection,
regardless of whether they believe that their sex partners were successfully
treated.
Infants infected with chlamydia
may develop conjunctivitis (infection of the membrane lining the eyelids)
and/or pneumonia. Chlamydial infection in infants can be treated with
antibiotics.
What about partners?
If a person has been diagnosed
and treated for chlamydia, he or she should tell all anal, vaginal, or oral sex
partners from the past 2 months so that they can see a healthcare provider and be
treated. This will reduce the risk that the sex partners will develop serious
complications from chlamydia and will also reduce the person’s risk of becoming
re-infected. A person with chlamydia and all of his or her sex partners must
avoid having sex until they have completed their treatment for chlamydia (i.e.,
seven days after a single dose of antibiotics or until completion of a
seven-day course of antibiotics) and until they no longer have symptoms. For
tips on talking to partners about sex and STD testing, visit www.gytnow.org/talking-to-your-partner/![]()
To help get partners treated
quickly, healthcare providers may give patients extra medicine or prescriptions
to give to their sex partners. This is called expedited partner therapy or EPT. EPT is
only available in some parts of the country. Consult a healthcare provider to
find out if it is available in a specific area. Sex partners should still be
encouraged to see a healthcare provider, regardless of whether they receive
EPT.
How can chlamydia be prevented?
Latex male condoms, when used consistently and correctly, can reduce the risk of getting or giving chlamydia. The surest way to avoid chlamydia is to abstain from vaginal, anal, and oral sex or to be in a long-term mutually monogamous relationship with a partner who has been tested