WUNRN
The
Lancet, Volume
379, Issue 9822, Pages 1225 - 1233, 31 March 2012
Log in required, but article free.
EQUITY IN MATERNAL, NEWBORN &
CHILD HEALTH INTERVENTIONS IN COUNTDOWN TO 2015: A REVIEW OF SURVEY DATA
FROM 54 COUNTRIES
Summary
Background
Countdown
to 2015 tracks progress towards achievement of Millennium Development Goals
(MDGs) 4 and 5, with particular emphasis on within-country inequalities. We
assessed how inequalities in maternal, newborn, and child health interventions
vary by intervention and country.
Methods
We
reanalysed data for 12 maternal, newborn, and child health interventions from
national surveys done in 54 Countdown countries between Jan 1, 2000, and Dec
31, 2008. We calculated coverage indicators for interventions according to
standard definitions, and stratified them by wealth quintiles on the basis of
asset indices. We assessed inequalities with two summary indices for absolute
inequality and two for relative inequality.
Findings
Skilled
birth attendant coverage was the least equitable intervention, according to all
four summary indices, followed by four or more antenatal care visits. The most
equitable intervention was early initation of breastfeeding. Chad, Nigeria,
Somalia, Ethiopia, Laos, and Niger were the most inequitable countries for the
interventions examined, followed by Madagascar, Pakistan, and India. The most
equitable countries were Uzbekistan and Kyrgyzstan. Community-based
interventions were more equally distributed than those delivered in health
facilities. For all interventions, variability in coverage between countries
was larger for the poorest than for the richest individuals.
Interpretation
We
noted substantial variations in coverage levels between interventions and
countries. The most inequitable interventions should receive attention to
ensure that all social groups are reached. Interventions delivered in health
facilities need specific strategies to enable the countries' poorest
individuals to be reached. The most inequitable countries need additional
efforts to reduce the gap between the poorest individuals and those who are
more affluent.
Funding
Bill
& Melinda Gates Foundation, Norad, The World Bank.
Introduction
Countdown
to 2015 for maternal, newborn, and child survival was conceived in 20031
to track country and global progress towards achievement of Millennium
Development Goals (MDGs) 4 (reduce child mortality) and 5 (improve maternal
health).2 Countdown monitors
population-based estimates of coverage for effective interventions in 75
countries with high rates or numbers of maternal or child deaths. Data for
coverage indicators are obtained from nationally-representative household
surveys.3 Since its inception, Countdown
has emphasised the need to address inequities in maternal and child health as a
key strategy to improve health and survival.4 Stratified analyses of key
coverage indicators by sex, wealth, maternal education, urban or rural residence,
and region of the country have been an essential part of Countdown reports,3, 5,
6
country profiles, and publications.2,7—9
We
report analyses of nationally-representative surveys available for 54 of the 75
Countdown countries. We aimed to identify which of 12 key maternal, newborn,
and child health interventions are most inequitably distributed within these
countries and which were least likely to be equitable in the delivery of these
interventions. Furthermore, we assessed whether intercountry variability in coverage
is greater for poor than for richer individuals.
Methods
Data sources
We
used data from Demographic Health Surveys (DHS) and Multiple Indicator Cluster
Surveys (MICS) done in countries monitored by Countdown to 2015. We selected
the latest survey available for each country (as of October, 2010) that
included assessments of household wealth and calculations of a standard wealth
index, with exclusion of the countries with no survey or with a survey done
before 2000. Therefore, we included 54 countries in the analyses, of which 11
had surveys that were done between 2000 and 2004, 33 in 2005 or 2006, and ten
in 2007 or 2008. Of the remaining 21 Countdown countries, 15 had not done
either survey, four had done a survey before 2000, and two had no data for
household assets.
Selection of
indicators
We
selected a subset of intervention coverage indicators that together represent
all stages of the continuum of care for maternal and child health. We aimed to
include interventions with high and low coverage, and those delivered via
health services, the community, and mass education campaigns (table 1, appendix). Most coverage indicators are dependent on short recall
periods and were studied for all children younger than 5 years. For antenatal
care, skilled birth attendant, and early of breastfeeding, MICS provided
information for children born in the 2 years before the survey and DHS for
those born up to 3 years before the survey, even when the survey had data for
the 5 years before the survey.
Table
1Table image![]()
Magnitude
of inequalities by intervention in countries with available information
As
an overall indicator of intervention coverage we used a weighted mean of the
coverage of eight interventions (appendix) selected from four specialties (family planning,
maternity care, child immunisation, and case management). Boerma and colleagues9 proposed this indicator to
provide a summary measure of coverage that could be used to assess and report
equity in the context of multicountry and time-trend analyses. We refer to this
index as the composite coverage index, calculated as:
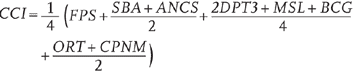
where
FPS is family planning needs satisfied, SBA is skilled birth attendant, ANCS is
antenatal care with skilled provider, DPT3 is three doses of Diphtheria,
Pertussis, and Tetanus (DPT) vaccine, MSL is measles immunisation, ORT is oral
rehydration therapy for children with diarrhoea, and CPNM is care seeking for
pneumonia. We assessed the composite coverage index to convey an overall
measure for the 12 interventions studied. We included the proportion of
children aged 12—23 months who received a dose of BCG vaccine in the index, but
did not assess this intervention separately. We calculated all indicators from
the original survey data, according to the standard definitions used by
Countdown3 (appendix). For all calculations we took into account the survey
design, including sampling weights and clustering. To verify the accuracy of
the calculations we checked global results for each indicator and country
against published results.
Equity analyses
For
the equity analyses, we used the wealth index scores for each household as
calculated by the original DHS or MICS survey team.10
These scores are presented in quintiles, with quintile 1 (Q1) representing the
poorest 20% of households in the survey sample and quintile 5 (Q5) representing
the richest. We calculated two absolute indicators of inequality (the difference
between Q5 and Q1, and the slope index of inequality) and two relative
inequality indicators (the ratio of Q5 to Q1, and the concentration index).
Because these indicators are proportions, we estimated the slope index of
inequality11
with logistic regression rather than with the traditional linear regression
approach to avoid predicting values in the regression model that were outside
the interval between 0 and 1. The slope index uses the coverage values in the
five quintiles to estimate the absolute difference in percentage points between
individuals at the top and bottom of the wealth scale. We calculated the concentration
index in its relative formulation, with no corrections.12 The concentration index is
expressed in a scale ranging from −100 to 100; a value of 0 represents
perfect equality, whereas positive values indicate that rich individuals have
greater coverage than do poor individuals.12
Seven
countries had no data for family planning needs satisfied. For these countries,
we imputed this indicator for each wealth quintile to allow calculation of the
composite coverage index. In the five countries with data for contraceptive
prevalence, we used Boerma and colleagues'9 approach in which family planning
needs satisfied is estimated from a linear regression model with contraceptive
prevalence as the predictor (correlation between family planning needs
satisfied and contraceptive prevalence was 0·97). In the other two countries,
we imputed family planning needs satisfied from a linear regression model with
seven indicators that were available for all countries as predictors (oral
rehydration therapy, care seeking for pneumonia, skilled birth attendant,
antenatal care with skilled provider, DPT immunisation, measles vaccination,
and BCG vaccination, whose correlations with family planning needs satisfied
varied from 0·24 to 0·49). To avoid imputation of proportions outside the 0—1
interval, we applied the logit transformation to all variables before fitting
the regression models. We then calculated the composite coverage for each
wealth quintile and country with the data originally available, plus the
imputed values for family planning needs satisfied.
Statistical
analysis
We
did all analyses with publicly available data from national surveys. Ethics
procedures were the responsibility of the institutions that commissioned,
funded, or administered the surveys. We used STATA (version 11.2) for all the
analyses, taking into account the sampling design characteristics of each
survey.
Role of the funding
source
The
sponsors of the study had no role in study design, data collection, data
analysis, data interpretation, or writing of the report. The corresponding
author had full access to all the data in the study and had final
responsibility for the decision to submit for publication.
Results
Table 1 shows the mean values and IQRs for the measures of
inequality in all countries for which data were available. We presented the IQR
instead of SDs with means because the numbers were small and distributions
skewed. Data for coverage of nine of the 12 interventions were available for
all 54 Countdown countries. Data for use of insecticide-treated bednets for the
prevention of malaria were available only for countries with endemic malaria;
data for four or more antenatal care visits were available for the 37 countries
for which the data source was a DHS.
Table 1 and figure 1 show mean values of intervention coverage and summary
equity indices for the 54 countries. For eight of the 12 interventions, mean
overall coverage was between 40% and 60% (table 1). Children sleeping under an insecticide-treated bednet
was the only indicator with a mean coverage of less than 40%, whereas DPT
immunisation, measles vaccination, and antenatal care with a skilled provider
had coverage of greater than 60% (appendix p 3).
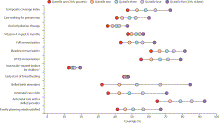
Figure
1 Full-size image (69K) Download
to PowerPoint
Mean
coverage in each wealth quintile for the studied interventions in 54 Countdown
countries
Coloured
dots show the average coverage in each wealth quintile. Q1 is the 20% poorest
wealth quintile; Q5 is the 20% richest. The distance between quintiles 1 and 5
represents absolute inequality. *Appendix p 1 specifies age ranges of children.
The
appendix shows the mean levels of intervention coverage against those of the
concentration index (relative inequality) and the slope index (absolute
inequality). We noted wide variability in inequities for skilled birth
attendant and vitamin A coverage despite similar levels of overall coverage (appendix p 3). Coverage of insecticide-treated bednets was the
only indicator with substantial variability between the absolute and relative
inequality findings.
Coverage
of skilled birth attendants was the least equitable of the 12 interventions,
according to all four summary indices (table 1). Mean national coverage for the 54 countries was 54%, but
the mean coverage in the poorest quintile was only 32%, compared with 84% in
the richest quintile (table 1). Antenatal care with a skilled provider had the highest
overall coverage of all indicators studied and moderate levels of inequity;
whereas, four or more antenatal care visits had much lower coverage and higher
inequity (table 1), despite the fact that the indicator does not need a
skilled provider. For all four summary indices, four or more antenatal care
visits was the second most inequitable indicator, surpassed only by skilled
birth attendant (table 1). When the analyses were limited to the 37 countries for
which four or more antenatal care visits were available, results for antenatal
care with a skilled provider remained unchanged compared with the first set of
results (data not shown). Antenatal care with a skilled provider was ranked
third of all 12 indicators for absolute inequality (SII and Q5—Q1 difference),
but was ranked sixth for relative inequalities (concentration index and Q5:Q1
ratio). Family planning was the third most inequitable intervention. Its
overall coverage was similar to that for skilled birth attendant, but its
coverage in the wealthiest quintile was modest compared with the other
indicators (table 1, figure 1). DPT immunisation and measles vaccination had high
coverage and intermediate levels of inequity, which we also noted for full
immunisation despite its lower coverage (table 1). Insecticide-treated bednets had a unique combination of
very low coverage, high relative inequity, and low absolute inequity (table 1; appendix). The low absolute inequity can be explained by the low
mean coverage in the wealthiest quintile; however, very low coverage in the
poorest quintile led to high relative inequality, even though coverage in the
richest quintile was also low. Early initiation of breastfeeding was by far the
most equitable indicator (table 1). It was the only intervention that, in a few countries,
had higher coverage in poor individuals than in rich, as shown by negative
values of the concentration and slope indices (table 1). Oral rehydration therapy and vitamin A were fairly
equitable, with moderate coverage (table 1).
Because
we derived the composite coverage index from several of the indicators, its
equity is within the range of values shown in table 1
and figure 1.
To assess which countries are least equitable, we compared concentration
indices for selected coverage indicators. We used coverage with skilled birth
attendant because it is dependent on strong health systems, and because it is
the most inequitable of all indicators studied. We used measles immunisation
coverage as an example of a moderately equitable indicator, perhaps because it
is often delivered through mass campaigns and needs one dose. We also assessed
the composite coverage index because it conveys an overall measure for the 12
interventions studied.
Country
ranks in inequalities (from high to low) varied according to the coverage
measure used (table 2).
Spearman rank correlation coefficients between the three indicators were all
positive (data not shown), which indicates that greater inequality in one
indicator was associated with greater inequality in all others. The lowest
correlation was 0·42 (skilled birth attendant vs measles vaccination),
followed by 0·72 (composite coverage index vs measles vaccination), and
0·75 (composite coverage index vs skilled birth attendant).
Nevertheless, we noted some consistent patterns when we used the information
about the three indicators simultaneously. Chad, Nigeria, Somalia, Ethiopia,
Laos, and Niger were clearly the countries with the largest inequalities,
closely followed by Madagascar, Pakistan, and India (figure 2). We noted the smallest inequalities for Uzbekistan and
Kyrgyzstan (figure 2).
Country rankings were very similar when we used the slope index of inequality
instead of the concentration index, except for countries with very low coverage
in the poorest individuals (eg, Somalia, Niger, Chad, and Ethiopia), which were
more equal according to the slope index than the concentration index (data not
shown). We investigated whether intervention coverage showed greater
variability in mothers and children from the poorest quintile than in those
from the wealthiest quintile each of the 54 countries. In figure 3, box plots show between-country variability in coverage
for skilled birth attendant, measles vaccine, and composite coverage index in
Q1 and Q5. As expected, median values for variability between countries in
coverage for skilled birth attendant, measles vaccine, and composite coverage
index were higher for the richest (Q5) than for the poorest (Q1) quintile, but
the variability in Q5 was substantially lower than that in Q1 (figure 3).
This finding is shown by the wider IQRs in Q1 compared with Q5, and by the
wider amplitudes of the whisker lines. Findings for measles vaccine are the
most remarkable, with Q1 amplitude covering almost all variation in Q5, which
implies that measles coverage for Q1 in some countries is far higher than for
Q5 in others (appendix shows findings for individual countries). After ranking
of countries according to Q5 coverage, those with similar levels of Q5 coverage
often had very different levels of Q1 coverage (appendix).
Table
2Table image![]()
Country
ranking according to the concentration index of selected indicators for 54
Countdown countries
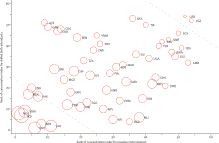
Figure
2 Full-size image (89K) Download
to PowerPoint
Scatterplot
of country ranks of inequality for skilled birth attendance and measles
immunisation
Circle
radii are proportional to the concentration index of the composite coverage
index for the 54 countries; large circles indicating more inequality. Country
codes are International Organization for Standardization country codes (appendix).

Figure
3 Full-size image (24K) Download
to PowerPoint
Box-plots
showing intercountry variability in the coverage of selected interventions in
the poorest and richest quintiles
Boxplots
do not show extreme or outside values that are detached from the data
distribution shown by the whisker lines.
With
some exceptions (eg, skilled birth attendant in Burkina Faso and measles in
Tajikistan), we noted monotonic increases in coverage with wealth quintiles (appendix pp 4—6). Inequalities in skilled birth attendant coverage
were much greater than were disparities in measles immunisation (appendix pp 4—6). Inequalities in the composite coverage index
were between these two indicators (appendix pp 4—6), which was expected because it represents an
average of indicators of maternal and child health.
Discussion
We
have described inequalities in intervention coverage. These inequalities seem
to be unfair and avoidable, and therefore represent inequities.13
Our first objective was to compare how different coverage indicators perform in
terms of equity. Our findings show that interventions with similar levels of
overall coverage often have very different degrees of inequality. The most
inequitable indicator was skilled birth attendant, followed by four or more
antenatal care visits, whereas the most equitable was early initiation of
breastfeeding. These analyses confirm previous findings that, unlike in
high-income countries, in many low-income countries, breastfeeding is more
prevalent in poor than in rich individuals.3,14—16 Notably, despite low overall coverage,
inequalities are small.
Interventions
that are usually delivered in fixed health facilities, particularly those that
need constant access to secondary-level or tertiary-level care, tend to be the
most inequitably distributed in the population.3, 17
Furthermore, the organisation and location of health facilities affects equity18 (eg, skilled birth attendant and
four or more antenatal care visits). Interventions that are often delivered at
community level (eg, vaccinations or vitamin A supplementation) tend to be much
more equitable than are those delivered in health facilities. Cost might also
be a factor. Some interventions are usually provided free of charge, such as
vaccinations and vitamin A, but others might need out-of-pocket spending by
families, either for services or because families need to travel to a health
facility. For example, in Uzbekistan, Kyrgyztstan, and Brazil,19
where maternity hospitals are accessible and free of charge, coverage for
skilled birth attendant is almost universal. Cultural perceptions might affect
care-seeking patterns and the choice of whether to adopt specific
interventions, such as contraceptives or breastfeeding, despite counselling or
information campaigns.
Countries
with similar levels of overall coverage often had very different results for
equity. Systematic analyses of the reasons for success in equitable countries
are important to understand their achievements and to transfer their
experiences to other countries with greater inequities. Several promising
approaches have been identified to improve equity, including deployment of
services and health workers in the areas most in need, task shifting,
reductions in financial barriers to access to services, and conditional cash
transfers (panel).18,22—24
Panel
Research
in context
Systematic
review
Our
findings add to international comparisons of intracountry inequalities in child
health and nutrition published in the past decade,4, 20,
21
and to those from a systematic review on this topic.23
Studies published between Jan 1, 1990, and Dec 31, 2010, were identified with
PubMed with several keyword combinations of “socioeconomic factors” with terms
related to child morbidity, mortality, nutrition, use of services, and
coverage. The search was restricted to publications about low-income and
middle-income countries, or global analyses.
Interpretation
Previous
publications did not include the most recent surveys done in low-income and
middle-income countries, or provide systematic analyses of which countries have
the highest inequalities or which interventions are most inequitably
distributed.
With
new analyses of recently available Demographic and Health Surveys and Multiple
Indicator Cluster Surveys, we showed that delivery by a skilled birth attendant
and antenatal care visits (more than four) had the greatest socioeconomic
inequalities. We identified which countries of those with existing data had the
widest inequalities. We related the degree of inequality to the delivery of
interventions, thus identifying those traditionally provided by health
facilities as the most inequitable compared with those delivered by outreach or
mass campaigns. Intercountry variability in intervention coverage is much
greater for the poorest wealth quintile in each country than for the richest,
which suggests that even in the poorest countries, wealthier individuals have
mechanisms for gaining access to lifesaving interventions.
Immediate
implications of our results include the need to give special attention,
nationally, regionally, and internationally, to the most inequitable
interventions. Community-based interventions were generally more equally
distributed than were service-based interventions, which indicates that
additional efforts are needed to reach the poorest individuals with such
interventions. The most inequitable Countdown countries need renewed efforts
from the international community.
The
choice of indicator is important when inequalities are assessed—eg, antenatal
care with a skilled provider and four or more antenatal care visits had
different levels of coverage and magnitude of inequalities. Aggregated coverage
measures, such as the composite coverage index, might mask the different
patterns of coverage and inequality noted for single-intervention coverage indicators.
However, these indicators are less affected by sampling variability and allow
for a more simple comparison of countries than would be possible if several
indicators were used. The indicators used should be appropriate for the
questions being addressed; aggregate measures could be useful for some
purposes, such as global monitoring, but are less helpful in guiding policy and
programme decisions at country level than are single indicators.
We
compared the magnitude of inequalities across the 54 countries at the time of
the latest survey. Our findings show a clear pattern with five highly
inequitable counties in the northern half of sub-Saharan Africa: Nigeria,
Niger, Chad, Ethiopia, and Somalia. Additionally, Madagascar, Laos, India, and
Pakistan were similarly inequitable. The most equitable countries were
Uzbekistan, Kyrgyzstan, Egypt, Malawi, Swaziland, and Tajikistan. Because
country rankings varied according to each coverage indicator used, and to
whether we used relative or absolute measures of inequality, these results
should be interpreted with caution.
Variability
between countries was substantially greater in individuals in the poorest
quintile than in those in the richest, which suggests that irrespective of how
poor a country is, those in the richest quintile have the means to ensure
fairly high coverage levels to mothers and children. Many individuals in the
richest quintile of most countries live in urban areas, which could partly
explain why they have increased access to the interventions. How much of these
differences are attributable to area of residence or region is an issue that we
will assess in future publications. Our findings add to those of previous
analyses of survey data from Countdown countries.9
Comparisons of survey results from several countries might be affected by
methodological differences—eg, although both MICS and DHS are standardised
across countries, DHS achieve a higher level of standardisation. Furthermore,
some discrepancies exist between the two sets of surveys—eg, variables related
to pregnancy and delivery are reported for children born in the past 2 years
for MICS, and the past 3 years for DHS. We used the most recent survey for
which the dataset was publicly available by October 2010, but questions about
the quality of some surveys remain. For example, socioeconomic variation in
skilled birth attendant coverage in Burkina Faso was unexpectedly small in the
2006 MICS (slope index of inequality equal to 2·3 percent points; appendix), but the same index was much wider in the 2003 DHS
(equal to 63·2 percent points).
Although
the assessment of socioeconomic position on the basis of asset indices might be
affected by the choice of assets and poor comparability between urban and rural
areas,25,
26
such indices are easy to compute and compare well with more complex indicators
of wealth.27—29
The usefulness of asset indices for discrimination of different subpopulations
is evident by their strong association with most coverage indicators. However,
wealth quintiles are specific to a given country, and the poorest quintile in a
middle-income country might be wealthier than the third or fourth quintile in an
extremely poor country. Furthermore, irrespective of the actual magnitude of
intracountry differences in wealth between rich and poor individuals, all
samples will be represented as five groups with about 20% of all households
each. Despite these limitations, use of asset indices allows the systematic
comparison of inequalities in health that would not be possible with other
measures of socioeconomic position. The coverage indicators that we used in the
analyses are based on maternal recall, and further work is being done to assess
and improve their validity. In addition to non-differential recall, which could
dilute any existing associations, some indicators might be affected by
differential reporting by rich and poor mothers, thus leading to bias.
Another
potential source of bias is that surveys were done over 8 years and secular
changes in inequalities might have occurred. However, the correlation between
the year of the survey and the concentration indices for the three main
coverage indicators (composite coverage index, skilled birth attendants, and
measles vaccine) were all between 0·1 and −0·1. Additionally, we noted no
significant associations between the type of survey and these three
concentration indices (data not shown). A potential caveat of the composite
coverage index is its reliance on arbitrary weights, giving equal weights to
four domains (family planning, pregnancy and delivery care, immunisations, and
case management of childhood illness). However, when we included these eight
separate indicators in a principal components analysis (appendix),
the first component shows a correlation coefficient of 0·95 with the composite
coverage index, suggested that the arbitrary weights did not affect the
resulting index.
We
make a clear distinction between absolute and relative inequality, because the
choice of indicators might affect the interpretation of findings.30—32
In several situations, especially when change in inequalities are assessed,
absolute and relative indicators might lead to conflicting findings.
Furthermore, the indices showing the difference and ratio of coverage levels in
Q1 and Q5 are simple measures that are easy to understand. However, the
concentration index and the slope index of inequality are more complex, but
account for the whole distribution, rather than only the richest and poorest
quintiles. We therefore used all four indices, but with emphasis on relative
inequality with the concentration index.
Concern
about inequalities in maternal and child health in poor countries was
conspicuously absent from the global agenda in the past,4
but has gained increased attention. UNICEF33
and the Commission on Information and Accountability for Women's and Children's
Health now emphasise equity as a priority.34
At the same time, the increase in the number of available surveys in low-income
and middle-income countries3
allows for international comparisons that were not feasible only a few years
ago. Countdown to 2015 is producing continuous analyses of national surveys to monitor
inequalities in coverage of cost-effective interventions, and providing regular
feedback to policy makers and health managers at country level. Because health
services often contribute to aggravation of health inequalities in35
mainstreaming of equity considerations into health policies and programmes can
contribute to the achievement of national and international health goals.
Contributors
All
authors participated in discussions about the data sources and planning of
analyses, and have critically revised versions of the report. AJB and CGV
conceived the study, did the analyses, and prepared the draft report. All
authors have seen and approved the revised version of this report.
Conflicts
of interest
We
declare that we have no conflicts of interest.
Acknowledgments
The
study was funded by the Bill & Melinda Gates Foundation, Norad, and the
World Bank.
WebExtra Content
Supplementary
appendix
PDF (158K)
References
1
The Bellagio Study Group on Child Survival. Knowledge into
action for child survival. Lancet 2003; 362: 323-327. Summary | Full
Text | PDF(91KB) | CrossRef | PubMed
2
BhuttaZAChopraMAxelsonH. Countdown to
2015 decade report (2000—10): taking stock of maternal, newborn, and child
survival. Lancet 2010; 375: 2032-2044. Summary | Full
Text | PDF(629KB) | CrossRef | PubMed
3
Countdown to 2015. Tracking
progress in maternal, newborn and child health. 2010 report. http://www.countdown2015mnch.org/reports-publications/2010-report/2010-report-downloads.
(accessed Nov 17, 2011).
4
VictoraCGWagstaffASchellenbergJAGwatkinDClaesonMHabichtJ-P. Applying an equity lens to child health and mortality:
more of the same is not enough. Lancet 2003; 362: 233-241. Summary | Full
Text | PDF(119KB) | CrossRef | PubMed
5
Countdown to 2015. Maternal,
newborn, and child survival. 2008 report. http://www.countdown2015mnch.org/reports-publications/2008report/2008reportdownloads.
(accessed Nov 17, 2011).
6
Countdown to 2015. Maternal,
newborn, and child survival. 2005 report. http://www.countdown2015mnch.org/reports-publications/2005report/2005reportdownloads.
(accessed Nov 17, 2011).
7
BryceJVictoraCG. Child survival: countdown to 2015. Lancet 2005; 365: 2153-2154. Full
Text | PDF(43KB) | CrossRef | PubMed
8
BryceJTerreriNVictoraCG. Countdown to
2015: tracking intervention coverage for child survival. Lancet 2006; 368: 1067-1076. Summary | Full
Text | PDF(472KB) | CrossRef | PubMed
9
BoermaJTBryceJKinfuYAxelsonHVictoraCG. Mind the gap: equity and trends in coverage of
maternal, newborn, and child health services in 54 Countdown countries. Lancet 2008; 371: 1259-1267. Summary | Full
Text | PDF(247KB) | CrossRef | PubMed
10
RutsteinSOJohnsonK. DHS comparative reports No 6: the DHS wealth index.
http://www.childinfo.org/files/DHS_Wealth_Index_(DHS_Comparative_Reports).pdf.
(accessed Nov 17, 2011).
11
MackenbachJPKunstAE. Measuring the magnitude of socio-economic inequalities
in health: an overview of available measures illustrated with two examples from
Europe. Soc Sci Med 1997; 44: 757-771. CrossRef | PubMed
12
KakwaniNWagstaffAvan DoorslaerE. Socioeconomic inequalities in health: measurement,
computation and statistical inference. J
Econ 1997; 77: 87-103. PubMed
13
WhiteheadM. The concepts and principles of equity and health.
Int J Health Serv 1992; 22: 429-445. CrossRef | PubMed
14
TrusselJGrummer-StrawnLRodriguezGVanlandinghamM. Trends and differentials in breastfeeding behaviour:
evidence from the WFS and DHS. Popul Stud 1992; 46: 285-307. PubMed
15
BarrosFCVictoraCGScherpbierRGwatkinD. Socioeconomic inequities in the health and nutrition of
children in low/middle income countries. Rev
Saude Publica 2010; 44: 1-16. CrossRef | PubMed
16
LiRGrummer-StrawnL. Racial and ethnic disparities in breastfeeding among
United States infants: Third National Health and Nutrition Examination Survey,
1988—1994. Birth 2002; 29: 251-257. CrossRef | PubMed
17
HouwelingTARonsmansCCampbellOMKunstAE. Huge poor-rich inequalities in maternity care: an
international comparative study of maternity and child care in developing
countries. Bull World Health Organ 2007; 85: 745-754. PubMed
18
BarrosAJDVictoraCGCesarJANeumannNABertoldiAD. Brazil: are health and nutrition programs reaching the
neediest?. In: Gwatkin DR, Wagstaff A, Yazbeck AS, eds. Reaching the
poor with health, nutrition, and population services: what works, what doesn't,
and why. Washington,
DC: World Bank, 2005: 281-306.
19
BarrosAJSantosISBertoldiAD. Can mothers rely on the Brazilian health system for
their deliveries? An assessment of use of the public system and out-of-pocket
expenditure in the 2004 Pelotas Birth Cohort Study, Brazil. BMC Health Serv Res 2008; 8: 57. CrossRef | PubMed
20
BoermaJTBryceJKinfuYAxelsonHVictoraCG. Mind the gap: equity and trends in coverage of
maternal, newborn, and child health services in 54 Countdown countries. Lancet 2008; 371: 1259-1267. Summary | Full
Text | PDF(247KB) | CrossRef | PubMed
21
GwatkinDRRutsteinSJohnsonKSulimanEWagstaffAAmozouA. Socio-economic differences in health, nutrition, and
population within developing countries: an overview. http://siteresources.worldbank.org/INTPAH/Resources/IndicatorsOverview.pdf.
(accessed Nov 17, 2011).
22
HosseinpoorARVictoraCGBergenNBarrosAJBoermaT. Towards universal health coverage: the role of
within-country wealth-related inequality in 28 countries in sub-Saharan Africa.
Bull World Health Organ 2011; 89: 881-890. CrossRef | PubMed
23
BarrosFCVictoraCScherpbierRGwatkinD. Health and nutrition of children: equity and social
determinants. In: Blas E, Kurup AS, eds. Equity, social determinants, and public health
programmes. Geneva, Switzerland: World Health Organization, 2010: 49-76.
24
LagardeMHainesAPalmerN. Conditional cash transfers for improving uptake of
health interventions in low- and middle-income countries: a systematic review.
JAMA 2007; 298: 1900-1910. CrossRef | PubMed
25
MorrisSSCarlettoCHoddinottJChristiaensenLJM. Validity of rapid estimates of household wealth and
income for health surveys in rural Africa. J Epidemiol Community Health 2000; 54: 381-387. PubMed
26
HouwelingTAKunstAEMackenbachJP. Measuring health inequality among children in
developing countries: does the choice of the indicator of economic status
matter?. Int J Equity Health 2003; 2: 8. PubMed
27
HoweLDHargreavesJRHuttlySR. Issues in the construction of wealth indices for the
measurement of socio-economic position in low-income countries. Emerg Themes Epidemiol
2008; 5: 3. PubMed
28
FilmerDPritchettLH. Estimating wealth effects without expenditure data—or
tears: an application to educational enrollments in states of India. Demography 2001; 38: 115-132. CrossRef | PubMed
30
HouwelingTAKunstAEHuismanMMackenbachJP. Using relative and absolute measures for monitoring
health inequalities: experiences from cross-national analyses on maternal and
child health. Int J Equity Health 2007; 6: 15. PubMed
31
MoserKFrostCLeonDA. Comparing health inequalities across time and place—rate
ratios and rate differences lead to different conclusions: analysis of
cross-sectional data from 22 countries 1991—2001. Int J Epidemiol 2007; 36: 1285-1291. CrossRef | PubMed
32
Harper S, King NB, Meersman SC, Reichman ME, Breen N, Lynch J. Implicit value
judgments in the measurement of health inequalities. Milbank Q88:
4—29.
33
UNICEF. Progress for
children 2010: achieving the MDGs with equity. http://www.unicef.org/protection/Progress_for_Children-No.9_EN_081710.pdf.
(accessed Nov 17, 2011).
34
Commission on information and accountability
for Women's and Children's Health. Keeping promises, measuring results. Final report of
the Commission. http://www.who.int/topics/millennium_development_goals/accountability_commission/Commission_Report_advance_copy.pdf.
(accessed Nov 17, 2011).
a Postgraduate
Program in Epidemiology, Federal University of Pelotas, Pelotas, Brazil
b London School
of Hygiene and Tropical Medicine, London, UK
c Department of
Economics, Lund University, Lund, Sweden
d Partnership
for Maternal, Newborn, and Child Health, WHO, Geneva, Switzerland
e Department of
Measurement and Health Information Systems, WHO, Geneva, Switzerland
f UNFPA, New
York, NY, USA
g Department of
International Health, Johns Hopkins Bloomberg School of Public Health,
Baltimore, MD, USA




