WUNRN
UGANDA - WHEN NO ELECTRICITY,
MIDWIVES DELIVER BABIES
& REDUCE MORTALITY WITH LIGHT
OF MOBILE PHONES
A midwife from Katine village in
Madudu and her fellow
midwives regularly have to help mothers deliver using the light cast by mobile
phones, held in their mouths to ensure the beams are directed where needed.
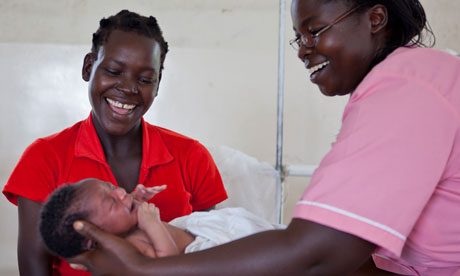
Midwife Esther
Madudu with Priscilla Alupo and baby George at Tiriri health centre, Katine.
Photograph: Steve Murigi/Amref
Priscilla
Alupo is propped up on a bed in Tiriri health centre's postnatal ward on a
sunny Saturday afternoon in Katine, north east Uganda. Her son, George, is lying
by her side. Alupo has a wide smile on her face as she shows him off to
visitors.
Esther Madudu, one of the health
centre's three midwives, helped deliver George the night before, during a
hectic 24-hour shift in which five babies were born. "Most babies are born
at night because they were made at night," jokes Madudu as she shows me
around the ward. From what she tells me, though, giving birth at night in a
health centre that has no electricity is anything but funny.
Madudu and her fellow
midwives regularly have to help mothers deliver using the light cast by mobile
phones, held in their mouths to ensure the beams are directed where needed.
The electricity supply to the health centre was cut by the Lord's Resistance Army during an attack on Katine eight years ago; it has yet to be restored. And the solar panels on the roof are broken. The centre does at least have mains water, and a borehole if that fails.
The mobile phones will probably
be needed again tonight. Jennifer Akajo is in one of the beds in the labour
ward, and Madudu – guided by a chart hanging on the wall next to her, which
estimates delivery time against dilation – predicts she's still got some way to
go. Akajo looks tired and nervous, but says little. Madudu gently rubs her
back; it's the only form of pain relief the centre can offer, she says.
Madudu, 31, has been a midwife
for 11 years and is clearly passionate about her work. "I grew up wanting
to be a midwife," she says. "I love talking about the mothers I help
deliver. We deliver 45 to 50 mothers every month, so I save 45 to 50 mothers
and babies a month." In the four years since she's been at Tiriri, no
mother has died in childbirth.
This week,
Madudu will be leaving Tiriri and heading to Deauville in France (her first
time out of Uganda), where she will address delegates at the Women's
Forum Global meeting, alongside Uganda's minister of health, Christine
Ondoa, and with the backing of Uganda's first lady, Janet Museveni. As well as
talking about her work and the health challenges faced by women, on Thursday
Madudu will launch the Stand Up for African Mothers campaign, organised by the African
Medical and Research Foundation (Amref). The NGO hopes its global campaign,
which will be fronted by Madudu, will draw attention to the continent's high maternal mortality
rates and advocate for ways to reduce it.
According to
UN estimates, around 358,000 women die in pregnancy or childbirth every year,
usually because they don't have access to basic medical care or trained staff
to help them deliver. The majority of the deaths in pregnancy – 280,000 – occur
in sub-Saharan Africa. Around 70% of African
women do not receive prenatal care and half of all deliveries take place at
home without any medical assistance. In
In its
report in April, Missing Midwives, the NGO Save the Children estimated that 350,000 more midwives are needed around the world to help reduce
maternal and child deaths. Without significant extra funds and effort, the
millennium development goals to cut death rates among women and children are
unlikely to be met in many countries by the 2015 deadline.
Amref, which
has been implementing a development project in Katine funded by Guardian readers and Barclays, hopes
its campaign will reduce the number of maternal deaths around the world by 25%.
It wants to train 30,000 midwives, including 10,000 in
The shortage of midwives and
healthcare workers is a particular problem in rural areas, such as Katine,
where low wages and inadequate housing make it hard to attract and retain
staff. Tiriri health centre has only recently managed to hire a doctor, and
another three midwives are needed to ease the burden on Madudu and her team.
"No one wants to be in rural
places," says Madudu, who over the next three years will travel the world
to promote the African mothers campaign. "But when you love your work and
want to save the lives of mothers, you go there. That's why I stay in Tiriri.
The pay is little, but God pays me because I know I have saved lives."
Joshua Kyallo, Amref country
manager for
Madudu says she is "very
glad" Amref chose her, and is quick to point out that her shifts will be
covered while she's away from Katine. "I feel good, I feel I am going to
share a lot of experiences and defend the fate of the mothers of Africa. I feel
we are going to save more mothers and babies.
"My dream was to save lives.
When you hear a baby cry on delivery, everyone begins to rejoice."