WUNRN
NEPAL - WOMEN'S JOURNEY TO FOOD
& HEALTH IN RURAL MUGU, NEPAL
By Jin Ju - Asian Human Rights
Commission AHRC
The blue sky is dazzling. Far off in the distance, being sharply shaken in a light airplane having only seven seats, passengers can see
beautiful snowy mountains on the right
side and the deep blue Rara lake on the left. Isolated villages are dotted
amongst the valleys. This is Mugu, the
most vulnerable and food insecure of

Two
helicopters arrived at about the same time as us, carrying rice from the World Food Program (WFP). Other women were waiting to
carry these 50kg parcels of rice, food
aid provided as a ‘work for food’
program. I wondered if the WFP was aware that a woman who may not eat enough
rice or other food items today, is carrying 50kg of rice. Since the WFP launched its food aid in
2008, had the WFP ever thought of making
a rice parcel smaller than 50 kilograms? Other women, regardless of their age,
stare at you. Carrying heavy loads on
their backs seems to be a punishment
given by God.
We tried to look for strong boys to carry our luggage, but ended up handing over them to women and girls. There were no boys; only
women and their daughters are willing to carry anything. We regretted not dividing our luggage in small bags. The biggest suitcase is given
to a 35-year-old woman, a mid-size bag
for her daughter, and a small bag for an old woman. The 35-year old-woman
wanted to carry all the luggage to earn more money, confidently saying, “I used to carry more than this, I can carry all. No
problem!” We suggested that for the price of three bags, she carry the biggest
one only.
It was a steep and sometimes rocky path to
the town of

Another
three to four hours by foot from the town is the Ruga village of the Ruga Village
Development Community (VDC), where 118 households live. Most of them belong to Dalit communities. Unlike Dalits living in
While high caste groups are also poor and deprived of basic resources and
rights, it is the Dalits who are the poorest in
Mugu. In Ruga, some high caste families and individuals share the same living condition as Dalits. Regardless of their
caste, all of them go to the temple together, and sit and chat together. There are some discriminatory
customs against women, a few of which are only
practiced by high caste villagers.
“Women wash their husbands’ hands and feet every morning and evening, and drink the water afterwards,” says one high caste
man for instance. A Dalit man
responds, “We don’t practice it, only they do.” They both laugh, as if it is
not a big deal. Sitting behind men, women say nothing. It is common practice for women to be kept in isolation after giving birth—for five days after the birth of a
son and 10 after the birth of a girl. Immediately after that, women go back to work. Women also have to stay at another place during their menstruation period. This is based
on the belief that women pollute the ‘sacred’ while performing anything
related to reproduction. Although this
practice is being disappeared in
“Did you bring medicines,” an old woman asked. When I said no,
she asked, “Why did you come here then?” In
fact, many women asked us if we had any medicine.
One old woman showed me her stomach,
asking for medicines for her stomachache and headache. I took out some herbal balm from my bag and
applied it to her forehead and around
her nose. What else could I do? The other women also asked me to apply the balm on their faces, which I
did one by one. They seemed happy with it. They also wanted contraception to control the frequency of pregnancy, which
they are unable to obtain. A few years back, some were given contraception
by a female foreign doctor funded by
an international agency, while others
obtained it from a Nepali male doctor. The former was used successfully
without any side effects, while the latter caused the women some discomfort. In accordance with their experience, the
women therefore now prefer female foreign doctors
for medical assistance.
.
Many women in the village have
suffered the death of their infants. A
33-year-old Dalit woman lost two children prior to the two she has now, the first at the age
of three months, and the second at six months. It is not difficult to understand why they died—her poor living condition provides her with insufficient nutrition, particularly during pregnancy. Rice and roti (local
wheat bread) are all that she eats. Even then, she cannot eat her preference of
locally produced rice, but only manages to
buy cheaper Japanese rice distributed by the Nepal
Food Corporation (NFC) at a subsidized
price. Most of the women suffer from vomiting
or breathing difficulties through the
consumption of Japanese rice. The women can only harvest a little local rice,
millet, wheat, or beans from their own land. It is particularly difficult to cultivate green vegetables and rice due to limited water resources; they are
completely dependant on rain.
Furthermore, this Dalit woman did not have a well-trained midwife who could help her during her labor at home. There are many cases
where a woman’s first or second child died early on. Another woman said she
lost five of her children, all of whom died of diarrhea. Eight to ten children are dying of diarrhea, pneumonia, or
malnutrition-related sicknesses every year, the women noted. They also observed
that their children get sick with vomiting
or diarrhea when they try to
breastfeed immediately after returning
from field work. The women assumed that it could be due to the hot temperature of their milk.
Additionally, the supplement nutrition powder distributed by the WFP does not
seem to suit the children. Women were
provided with three parcels of it, each containing
90 bags of 10 grams each in December
2010, to be fed to the children after being mixed with rice. As a result of consuming this however, the children suffered from
vomiting or diarrhea. Mothers who
visited the District Health Centre
(DHC) were given free medicines, but
complained that the medicines were bad. This reflects the DHC’s lack
of credibility, and that women are not instructed
how to keep the medicines properly.
Despite all the problems women face, no one consults with them and nothing is accurately reported. One can assume
that the situation of remote areas must be worse than found in Ruga village.
The health worker attached to the health
post comes once a month to give polio injections to the children. At the District Health Centre, we met a senior Auxiliary
Nursing Midwife (ANM) Mrs Saroja
Chimire who has been working in Mugu
for the last 18 years. The other staff include
one senior health officer, one senior
midwife, two junior assistants who joined
last year, and one social health
worker from UNICEF. Only the two senior staff are from Mugu, the rest are from elsewhere. As the
officers only keep medical records of patients who come for treatment, no one
knows how many children or women die of water bone diseases or other sicknesses
associated with malnutrition. UNICEF Nepal
suggests that half of the country’s children are undernourished, and the local
staff of UNICEF Mugu asserts that 7-8
percent of the children are severely malnourished in Mugu.
However, there is no precise data presenting
the real picture.
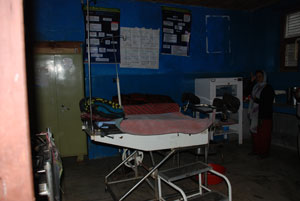
We saw a few patients lying in beds, and were told that some pregnant women give birth at
the DHC. When pregnant women visit the DHC four times a year, they are entitled
to 400 Nepali rupees (USD 5), while those who give
birth there get 1,500 Nepali rupees
(USD 20). The DHC health officers hold
seminars on mortality, pregnancy, and
nutrition targeting mothers. They aim to reduce mother mortality by encouraging mothers to come to
public health institutions for delivery or other medical
treatment. The biggest obstacle for women in
accessing such institutions is the total absence of transportation. It is
almost impossible for mothers who have serious medical issues to come to
the DHC on foot. For the same reason, mothers cannot bring their malnourished children to the DHC for treatment.
The
villagers of Ruga go to the DHC
located at the nearby headquarters instead
of the village health post farther
away, which requires five hours of walking
uphill to reach. Unless it is urgent,
villagers find it difficult to go to
the public health institutions. Even then, it takes a couple
of hours to reach from the villages
located near the headquarter zone, and some days to reach from the remote villages. Although
the medicines and treatments are free,
the physical distance is the biggest challenge. Furthermore, there has been no
doctor posted at the DHC for the past five
months; the previous doctor left for
personal reasons and no replacement doctor
has yet been posted. The patients who require surgery are referred to the hospital in Nepalgunj,
which the villagers have to fly to.
Not just medical officers, but all government officers working in
Mugu are from other districts. Their
term is very short, one to two years,
which means they leave before truly learning
about Mugu. The remote and undeveloped
nature of the district requires these officers to be paid compensation as an incentive, while their short term status
encourages them to engage in corruption. This causes further distress to young villagers; the village’s one
college bears 200 students every year, who find
it difficult to find jobs in
Mugu, while government and public jobs
are filled by external officers.
One good leader can make a considerable difference. The senior ANM’s daughter
who currently studies at a university in
We promised to support her, encouraging her to
do her best to be a doctor in
the future. One day, you will see a lovely and warm-hearted female doctor sitting
in the DHC office in Mugu
or walking around the remote villages
looking after the poor villagers who
need medical treatment. She will perhaps make the necessary changes for mothers
and children in Mugu.