WUNRN
Full Article is free, but The Lancet
requires registration to access.
The
Lancet, Volume
372, Issue 9655, Pages 2047 - 2085, 13 December 2008
Health Systems
and the Right to Health: An Assessment of 194 Countries
Summary
60
years ago, the Universal Declaration of Human Rights laid the foundations for
the right to the highest attainable standard of health. This right is central
to the creation of equitable health systems. We identify some of the
right-to-health features of health systems, such as a comprehensive national
health plan, and propose 72 indicators that reflect some of these features. We
collect globally processed data on these indicators for 194 countries and
national data for Ecuador, Mozambique, Peru, Romania, and Sweden. Globally
processed data were not available for 18 indicators for any country, suggesting
that organisations that obtain such data give insufficient attention to the
right-to-health features of health systems. Where they are available, the
indicators show where health systems need to be improved to better realise the
right to health. We provide recommendations for governments, international
bodies, civil-society organisations, and other institutions and suggest that
these indicators and data, although not perfect, provide a basis for the
monitoring of health systems and the progressive realisation of the right to
health. Right-to-health features are not just good management, justice, or
humanitarianism, they are obligations under human-rights law.
Introduction
December,
2008, marks the 60th anniversary of the Universal Declaration of Human Rights.1
The declaration provides the foundation for the international code of human
rights.2
This code gives an internationally agreed set of standards to guide and assess
the conduct of governments across a wide range of sectors and has a direct,
close bearing on medicine, public health, and the strengthening of health
systems.3
The
international code of human rights consists of legally binding international
components. Among the most important of these components for health systems are
the International Covenant on Economic, Social, and Cultural Rights (ICESCR)4, 5 and the Convention on the Rights of the Child
(CRC).6 Both these human-rights treaties
are legally binding for those countries that have ratified them. Most states
have ratified the ICESCR, and all but two (Somalia and the USA) have ratified
the CRC. The right of everyone to enjoy the highest attainable standard of
physical and mental health—sometimes known as the right to the highest
attainable standard of health or the right to health—is an integral part of
both of these international treaties. All countries have ratified one or more
binding treaty that includes the right to health, such as the International
Convention on the Elimination of All Forms of Racial Discrimination.7
Also, many countries include this right in their national constitutions.8
The Constitution of WHO,9 the Declaration of Alma-Ata,10 the Ottawa Charter for Health
Promotion,11
the Bangkok Charter for Health Promotion in a Globalized World,12
and other important documents agreed by the health community also recognise
this fundamental human right.
In
recent years, national and international policy makers, courts,
non-governmental organisations, and other stakeholders have adopted and applied
features of the right to the highest attainable standard of health. Uganda's
review of its health policy expressly uses a right-to-health analysis13
as does WHO in, for example, its publication on human rights, health, and
poverty reduction.14
Courts, too, are explicitly relying on the right to health in their decisions,
most recently in a landmark judgment of the Colombian Constitutional Court.15—19 On the basis of a detailed understanding of
the right to health, this court effectively ordered a phased restructuring of
the country's health system by way of a participatory and transparent process
based on current epidemiological information.20
Civil-society guides to the right to health are increasing in number, and many
civil-society organisations use these in their work.21—24
Both the UN General Assembly and Human Rights Council have discussed numerous
reports on the right to health, covering a wide range of issues, such as
neglected diseases,25 sexual and reproductive health,25
maternal mortality,26 mental disability,27 the Millennium Development Goals
(MDGs),28 medicines,26
and water and sanitation.29
Recognition
that a strong health system is an essential element of a healthy and equitable
society is growing. However, according to a recent WHO publication, health
systems in many countries are failing and collapsing.30 Too many health systems are
inequitable, regressive, and unsafe.30 WHO also confirms that
sustainable development, including achievement of the MDGs, depends on
effective health systems.30
As
with a fair court system, an effective health system is a core social
institution and, for this reason, crucially, both systems are protected by
human rights.31, 32
Although many human rights are important to a well-functioning court system,
the key one is the right to a fair trial.33
Through human-rights treaties, national laws and policies, judicial decisions,
and so on, the right to a fair trial has helped to identify the key features of
a fair court system, such as an independent judiciary and trials without undue
delay. The right to a fair trial has not only identified unfair judicial
processes but also led to welcome reforms in many countries.
By
analogy, the right to the highest attainable standard of health can help to
establish health systems that are reasonably equitable. However, to make this
happen, the right-to-health features of health systems need to be identified.
This process will take time, just as our understanding of the right to a fair
trial has developed over many years. Once identified, the right-to-health
features will not provide a neat blueprint or formula for a health system.
There will be many grey areas, just as there are in relation to the right to a
fair trial and court systems.34
The right to a fair trial does not provide detailed prescriptions, rather it
insists upon key principles, such as fairness, independence and impartiality,
and several important features that a court system must have if it is to be
fair. The right to health has a similar role.
Of
all the important human rights that bear upon health systems, the right to the
highest attainable standard of health is the cornerstone of both an effective
health system and the growing movement for health and human rights.35
In this
Report, we aim to assess the degree to which the health systems of 194
countries include some of the features that arise from the right to health. We
introduce the right to health and identify some of the right-to-health features
of health systems. These features are not just a matter of good management,
justice, or humanitarianism—they are a matter of human-rights law. We set out
our methods and their limitations and identify 72 indicators of right-to-health
features of health systems. We present some of the findings and results arising
from the data on the indicators, and discuss these data and make
recommendations for a range of stakeholders.
What is the right
to health?
The
right to the highest attainable standard of health encompasses medical care, access
to safe drinking water, adequate sanitation, education, health-related
information, and other underlying determinants of health;36 it includes freedoms, such as
the right to be free from discrimination and involuntary medical treatment, and
entitlements, such as the right to essential primary health care.36 Like other human rights, the
right to health has particular concern for disadvantaged people and
populations, including those living in poverty. The right to health requires an
effective, responsive, integrated health system of good quality that is
accessible to all.37
International
human-rights law recognises that the right to the highest attainable standard
of health cannot be realised overnight; it is expressly subject to both
progressive realisation and resource availability.4 Put simply, progressive
realisation means that a country has to improve its human-rights performance
steadily; if there is no progress, the government of that country has to
provide a rational and objective explanation. Because of their greater resource
availability, more is expected of high-income than of low-income countries.
However, the right to health also imposes some obligations of immediate effect,
such as non-discrimination,4
and the requirement that a state at least prepares a national plan for health
care and protection.36 Furthermore, the right to health
requires that there are indicators and benchmarks to monitor progressive
realisation36 and that individuals and
communities have opportunities for active and informed participation in health
decision making that affects them.36 Under international human rights
law, developed countries have some responsibilities towards the realisation of
the right to health in developing countries.36 Because the right to health
gives rise to legal entitlements and obligations, effective mechanisms of monitoring
and accountability are needed.36
Although
the right to health adds power to campaigning and advocacy, it is not just a
slogan, it has a concise and constructive contribution to make to health policy
and practice. Health workers can use the right to devise equitable policies and
programmes that strengthen health systems and place important health issues
higher up national and international agendas.37,
38
Medicine,
public health, and human rights have much common ground. To one degree or
another, each field stresses the importance of the underlying determinants of
health and good-quality medical care, looks beyond the health sector, struggles
against discrimination and disadvantage, demands respect for cultural
diversity, and attaches importance to public information and education.
The
right to health cannot be realised without the interventions and insights of
health workers; and the classic, long-established objectives of public health
and medicine can benefit from the newer, dynamic discipline of human rights. A
few enlightened people understood these relations when the WHO Constitution was
drafted in 19469
and when the Declaration of Alma-Ata was adopted in 1978,10 affirming the right to the
highest attainable standard of health.
However,
until recently, the right to health was only dimly understood and attracted
limited support from civil society or any other sector. The understanding and
practice of health and human rights has improved since the Alma-Ata conference.35,39—43
One vital part of this process has been a deepening understanding of the right
to health. But it was not until 2000 that an authoritative understanding of the
right to health emerged when the UN Committee on Economic, Social, and Cultural
Rights, working in close collaboration with WHO and many others, drafted and
adopted general comment 14.36
Although
neither complete, perfect, nor binding, general comment 14 is compelling and
groundbreaking. The comment shows a substantive understanding of the right to
health that can be made operational and improved in the light of practical
experience. The influence of Alma-Ata on general comment 14 is explicit and
clear. Although much more work is needed to grasp all the implications of the
right to the highest attainable standard of health, the general comment
confirms that the right cannot be dismissed as a rhetorical device. General
comment 14 provides a common right-to-health language for talking about health
issues and sets out a way of analysing the right to health, making it easier
for policy makers and practitioners to use.27Panel 1 summarises general comment 14, including the requirement
that health facilities and services be available, accessible, and culturally
acceptable.
Panel
1
Some
important points from general comment 14
Article
12 of the International Covenant on Economic, Social, and Cultural Rights very
briefly sets out the right to the highest attainable standard of health.
General comment 14 provides the UN Committee on Economic, Social, and Cultural
Rights' interpretation of article 12. Although not legally binding, the comment
is highly authoritative.
- Encompassing physical and mental health, the right to
health places obligations on governments in relation to health care and
the underlying determinants of health—these obligations include provision
of clean water, adequate sanitation, nutritious food, adequate shelter, education,
a safe environment, health-related information, and freedom from
discrimination.
- Governments have, for example, obligations regarding
maternal, child, and reproductive health; healthy natural and workplace
environments; the prevention, treatment, and control of diseases; health
facilities, services, and goods.
- Governments have an obligation to give particular
attention to marginal individuals, communities, and populations, creating
a need for as much disaggregation of data as possible.
- Within a country, health facilities, services, and
goods must be available in sufficient quantity, accessible (including
affordable) to everyone without discrimination, culturally acceptable (eg,
respectful of medical ethics and sensitive to gender and culture), and of good
quality.
- The right to health is subject to progressive
realisation and resource availability.
- Nonetheless, governments must take deliberate,
concrete, and targeted steps to ensure the progressive realisation of the
right as expeditiously and effectively as possible.
- However, core obligations are subject to neither
progressive realisation nor resource availability. Expressly taking into
account the Declaration of Alma-Ata, they include obligations to ensure
access to health facilities, goods, and services to everyone, including
marginal groups, without discrimination; to ensure everyone is free from
hunger; to ensure access to basic shelter, housing and sanitation, and an
adequate supply of safe and potable water; to provide essential drugs, as
defined under the WHO action programme on essential drugs; to ensure
equitable distribution of all health facilities, goods, and services; and
to adopt and implement a national public-health strategy and plan of
action, by way of a participatory and transparent process.
- The right to health requires opportunities for as much
participation as possible by individuals and communities in health-related
decision making.
- Governments have an obligation to ensure that non-state
stakeholders are respectful of the right to health (eg, do not
discriminate).
- Developed states, and others in a position to assist,
should provide international assistance and cooperation in health to
developing countries (eg, economic and technical assistance to help
developing countries fulfil their core obligations). All states “have an
obligation to ensure that their actions as members of international
organizations take due account of the right to health”.
- Monitoring, accountability and redress are essential.
Given progressive realisation, indicators and benchmarks are indispensable
if governments are to be held to account.
- The right to health is closely related to, and
dependent upon, numerous other human rights, such as the rights to life,
education, and access to information.
- In narrowly defined circumstances and as a last resort,
the enjoyment of some human rights may be interfered with to achieve a
public health goal. For example, quarantine for a serious communicable
disease, such as ebola fever, may, under certain circumstances, be
necessary for the public good, and lawful under human rights, even though
it limits an individual's freedom of movement.
The
right-to-health analysis can be used to identify and expose, for example, the
lack of available mental-health facilities properly serviced by trained staff.44 Health-related facilities and
services, including mental-health facilities with properly trained staff, must
be available in adequate number throughout a country. Of course, the need is
subject to resource availability: more and better facilities are required of
Canada than of Chad. Few nations, however, devote adequate funds to mental
health.44, 45
On a routine basis, mental-health facilities are neglected, workers untrained,
and patients uncared for.44 Poor mental health gives rise to
other profound problems, not least discrimination and stigmatisation, important
to the right to health.
The
test of availability can also be applied to harm-reduction initiatives.46
Provision of injecting drug users with comprehensive and integrated treatment,
counselling, and clean needles and syringes is good for public health, reduces
avoidable suffering, saves lives, and is cost-effective.47
An appropriate harm-reduction initiative is also a right-to-health initiative.
However, most countries do not provide harm-reduction services for people who
use drugs, and those that do, such as Sweden, provide a limited and scattered
service.48
The right to health requires all countries to have an effective, national,
comprehensive harm-reduction policy and plan, delivering essential services. A
high-income country such as Sweden is expected to provide more than the
essential services.
Health-related
facilities and services can be available within a country but inaccessible to
all those who need them. For example, access to essential medicines is an
indispensable part of the right to health with several dimensions.49 First, medicines must be
accessible in remote rural areas as well as in urban centres, which has major
implications for the design of medicine supply systems. Second, medicines must
be affordable to all, including those living in poverty, which has obvious
implications for funding and pricing arrangements. Third, given the fundamental
human-rights principles of non-discrimination and equality, a national
medicines policy must be designed to ensure access for disadvantaged
individuals and communities, such as women and girls, people living with
HIV/AIDS, elderly people, and people with disabilities. Because equal access is
not always secured by equal treatment, a state must sometimes take measures in
favour of disadvantaged people. As far as possible, data must be disaggregated
to identify marginalised groups and monitor their progress towards equal
access. Fourth, reliable information about medicines must be accessible to
patients and health workers so they can take well-informed decisions and use
medicines safely.
Health-related
facilities and services may be available and accessible but be insensitive to
culture and gender. For example, improving the access to sexual and
reproductive health care is not simply about scaling up technical interventions
or making them affordable. A Peruvian project that studied indigenous
communities with very high maternal mortality found an acute reluctance within
the population to use the health facilities offered by the state, partly
because they did not take account of local cultural conceptions of health and
sickness. In close consultation with the indigenous communities, culturally
sensitive facilities and services were introduced, such as sturdy ropes in
delivery rooms so that women could give birth squatting and gripping the rope,
as they were accustomed to. These changes led an increase in deliveries in
local health centres,50
and the success of these local initiatives helped to generate a corresponding
change in national health policy on deliveries in all primary health-care
facilities.51
Right-to-health
features of health systems
The
Declaration of Alma-Ata identifies some vital components of an effective health
system. The declaration is especially instructive because of its public-health,
medicine, and human-rights aspects (panel 2),
and it provides compelling guidance on the core obligations of the right to
health.36
Panel
2
The
Declaration of Alma-Ata (1978)
Principal
themes
- The importance of equity
- The need for community participation
- The need for a multisectoral approach to health
problems
- The need for effective planning
- The importance of integrated referral systems
- An emphasis on health-promotional activities
- The crucial role of suitably trained human resources
- The importance of international cooperation
Essential
health interventions
- Education concerning prevailing health problems
- Promotion of food supply and proper nutrition
- Adequate supply of safe water and basic sanitation
- Maternal and child health care, including family
planning
- Immunisation against major infectious diseases
- Prevention and control of locally endemic diseases
- Appropriate treatment of common diseases and injuries
- Provision of essential drugs
Other
attempts have been made to identify what constitutes a functioning health
system.52 WHO identifies six essential
building blocks that make up health systems: health services (medical and
public health); health workforce; health information system; medical products,
vaccines, and technologies; health financing; and leadership, governance, and
stewardship.30 Although debatable, these
building blocks provide a useful way of looking at health systems and can be
thought of as building blocks for the realisation of the right to health.
However, a health system might have all these building blocks but still not
serve human rights. For example, the system might include both medical care and
public health but not secure fair access, or there might be a health
information system but key data might not be suitably disaggregated.
A
major challenge for human rights is to apply or integrate the right to health
across the six building blocks. The right-to-health analysis provided by
general comment 14 has to be systematically and consistently applied to health
services, health workforce, health information, medical products, financing,
and stewardship—that is, all the elements that together constitute a
functioning health system. Panel 3
identifies some of the issues that arise when the right-to-health analysis is
applied to the second WHO building block—the health workforce. The
right-to-health analysis of availability, accessibility, cultural
acceptability, quality, participation, international assistance and
cooperation, monitoring and accountability, and so on, can also be applied to
health systems to identify some of the right-to-health features of health
systems, encompassing what health systems do (for example, providing access to
essential medicines and safe drinking water) and the way in which they function
(for example, transparently, in a participatory process, and without
discrimination). Health systems run the risk of being impersonal, top-down, and
dominated by experts, but the right to health places the wellbeing of
individuals, communities, and populations at the centre.53
Irrespective of which of the many definitions of a health system is used,30, 52, 54
all the following features should be part of any health system.
Panel
3
Some
issues arising when the right to health is applied to health workforces
- General comment 14 requires a comprehensive national
health plan (eg, paragraphs 43[6] and 55) encompassing human resources. So
is there an up-to-date plan for human resources in preventive, curative,
and rehabilitative health, encompassing physical and mental health?
- Is there a role for midlevel providers who can increase
access to health care, such as assistant medical officers and surgical
technicians, and public-health professionals?
- Are there outreach programmes for the recruitment of health
workers from marginalised communities and populations, such as indigenous
peoples, to reduce non-discrimination and improve respect for cultural
difference?
- Are effective measures in place to achieve a gender
balance among health workers in all fields to ensure equality,
non-discrimination, and respect for cultural difference?
- Because health-related services must be available in
sufficient quantity, subject to resource availability, are effective
measures in place to ensure that the number of domestically trained health
workers is commensurate with the health needs of the population?
- Is health information about the number of health
workers by category (eg, nurses and public health professionals)
collected, centralised, and made publicly available on a regular basis?
- Are human rights, including respect for cultural
diversity, as well as the importance of treating patients and others with
courtesy, a compulsory part of the training for all health workers?
- General comment 14 (paragraph 44[5]) requires appropriate
training for health personnel, so are opportunities for further
professional training in place for all health workers without
discrimination?
- Are health workers receiving domestically competitive
salaries as well as other reasonable terms and conditions of employment? A
lack of reasonable terms and conditions of employment, one of the causes
of the skills drain, is likely to undermine a health system
- Are incentives in place to encourage the appointment,
and retention, of health workers in underserved areas to improve access,
especially of marginal communities and populations?
Legal
recognition—Countries
should give recognition to the right to health in national law and by ratifying
relevant human-rights treaties.36 In some countries legal
provisions on the right to the highest attainable standard of health are
generating significant case law.55 For example, Hogerzeil and
colleagues56 analysed 71 court cases from 12
countries and concluded that in 59 cases access to essential medicines was
enforced through the courts as part of the right to health. Legal recognition
is just one of the first steps on a long and difficult journey to realising the
right to health. Without follow-up from social movements, health workers,
progressive government ministers and public officials, activist courts, and
international support, in addition to governmental respect for the rule of law,
legal recognition is likely to be an empty promise.
Standards—Although important, legal
recognition of the right to health is usually confined to a general formulation
that does not set out in any detail what is required of those with
responsibilities for health. For this reason, countries must not only recognise
the right to health in national law, but also ensure that there are more
detailed provisions clarifying what society can expect by way of health-related
services and facilities. For example, provisions are needed for quality and
quantity of drinking water, blood safety, essential medicines, the quality of
medical care, and so on. Such clarifications may be provided by laws,
regulations, protocols, guidelines, and codes of conduct. WHO has published
important standards on various health issues.57—59 Many others have also contributed; for
example, the Sphere Project provides minimum standards for responses to
disasters.60
Clarification is important for providers, so they know what is expected of them
and also for those for whom the service or facility is intended, so they know
what they can legitimately expect.
Participation—Health systems must also
include institutional arrangements for the active and informed participation in
strategy development, policy making, implementation, and accountability by all
relevant stakeholders, including disadvantaged individuals, communities, and
populations.36 Examples of such participation
include conferences to develop national health plans in Brazil and Peru; a
legislative requirement of Maori participation in New Zealand's District Health
Boards; village health teams in Uganda; and the participatory transfer of an
HIV/AIDS clinic from Médecins Sans Frontières to the Guatemalan Ministry of
Health.61
Participation improves health outcomes.62
Transparency—Tempered by the confidentiality
of personal data, this requirement applies to all those working in
health-related sectors, including countries, international organisations,
public—private partnerships, business enterprises, and civil-society
organisations.36 The Medicines Transparency
Alliance, funded by the UK Government, is an alliance of governments,
international agencies, pharmaceutical companies, and civil-society
organisations, committed to increasing transparency of information on the
quality, availability, and pricing of essential medicines in the public,
private, and non-profit sectors.63
Equity,
equality, and non-discrimination—Health systems must be accessible to all, including those
living in poverty, minority groups, indigenous people, women, children, people
living in slums and rural areas, people with disabilities, and other
disadvantaged individuals, communities, and populations.36 Additionally, health systems
must be responsive to the particular health needs of women, children,
adolescents, elderly people, and so on.36 Outreach programmes are needed
to ensure that disadvantaged people have the same access as more privileged
people. Several European governments, for example, have established Roma health
mediator programmes.64 As members of the Romani
community themselves, the mediators aim to improve community health by
mediating between patients and health workers during consultations and
communicating with Romani communities on behalf of the public health system.
Although the programmes have limitations, mediators have greatly assisted some
Romani.64
The
right-to-health principles of equality and non-discrimination are akin to the
health concept of equity. All three concepts have a social-justice component.
In some respects, equality and non-discrimination, being reinforced by law, are
more powerful than equity.65
For example, if a government or other body does not take effective steps to
tackle discrimination, it can be held to account and required to take remedial
measures.66,
67
Respect
for cultural difference—From
the right-to-health perspective, health systems must be respectful of cultural
difference.36, 38,
68
Health workers must be sensitive to issues of culture, ethnicity, and sex,
strategies must be in place to enable indigenous people to study medicine and
public health, and so on.69
Quality—All health-related services
and facilities must be of good quality.36 For example, water quality
regulations and standards consistent with the WHO guidelines for the quality of
drinking water should be in place.57
The good quality requirement also extends to the way patients and others are
treated: health workers must treat patients and others politely and with
respect. Because medicines may be counterfeit, states must establish
appropriate regulatory systems.49
In Nigeria, for example, there is evidence that the National Agency for Food
and Drug Administration and Control's dual strategy of strengthening the
regulatory environment, while encouraging intolerance of counterfeit drugs
through public enlightenment campaigns is improving medicine safety and
quality.70
Planning—Some important implications
arise from the right to health being subject to progressive realisation and
resource availability. The crucial importance of planning is recognised in the
Declaration of Alma-Ata,10
general comment 14,36 and elsewhere.71
States must have comprehensive national health plans, encompassing both the
public and private sectors, for the development of health systems; because the
plans have to be evidence-based, a situational analysis with disaggregated data
is needed before the plan is drafted. Health research and development should
also inform the planning process.72, 73
According
to general comment 14, the plan must include certain features, such as clear
objectives (and how these are to be achieved), timeframes, effective
coordination mechanisms, reporting procedures, a detailed budget, financing
arrangements (national and international), assessment arrangements, indicators
and benchmarks to measure achievement, and one or more accountability devices.36 Indicators and benchmarks are
already commonplace features of many health systems, but they rarely have all
the elements that are important from a human-rights perspective, such as
appropriate disaggregation.36
The
identification of indicators and benchmarks to measure the progressive
realisation of the right to health is a national and international process that
involves countries, international organisations, the UN Committee on Economic,
Social, and Cultural Rights, and others. A wealth of data is available at the
global level, some of which is highly relevant to the right to health. But are
international bodies making other data important to the right-to-health
perspective available? If not, countries may wrongly assume that these other
data, and the issues to which they relate, are less important. Many countries
look to UN bodies for technical assistance, ideas, and leadership. Whether or
not UN bodies are making data that are highly relevant to the right to health
available at a global level is an important issue.
A
fair, transparent, participatory, and inclusive process for prioritising
competing health needs is required—one that takes into account explicit
criteria, such as the wellbeing of those living in poverty, and not just the
claims of powerful groups with vested interests.72
The process of prioritisation should give particular attention to the core
obligations identified in general comment 14 because they are required of all
countries, whatever their stage of economic development.36 The list of core obligations is
illustrative rather than exhaustive (panel 1).74
One of the core obligations is to adopt and implement a national public health
strategy and plan of action, on the basis of epidemiological evidence,
addressing the health concerns of the whole population.36
Before
the finalisation of the plan, key elements must undergo impact assessment to
ensure that they are likely to be consistent with national and international
legal obligations, including those relating to the right to the highest
attainable standard of health.75 In addition, the present realisation
of the right to health must be maintained, although this might be waived in
exceptional circumstances.36
Progressive
realisation does not mean that a government is free to choose whatever measures
it wishes to take so long as they reflect some degree of progress. General
comment 14 requires that governments take deliberate, concrete, and targeted
steps to ensure progressive realisation as quickly and effectively as possible.36
Progressive
realisation, maximum available resources, and core obligations need closer
conceptual and operational attention. Some courts have rejected the idea of
core obligations and required that government policies are reasonable.76
Other courts have taken the same position as the UN Committee on Economic,
Social, and Cultural Rights in general comment 14 and found that some
health-related responsibilities are so fundamental that they are subject to
neither progressive realisation nor resource availability.15,
77
This position most closely matches the right to health: progressive realisation
is an important concept with a crucial role, but only up to the boundaries of
core obligations.
Referral
systems—Health
systems should have a mix of primary (community-based), secondary
(district-based), and tertiary (specialised) facilities and services, providing
a continuum of prevention and care.52 The system also needs an
effective process by which health workers assess whether patients will benefit
from additional services and patients are referred from one facility or department
to another. Referrals are needed between alternative health systems (eg,
traditional health practitioners) and mainstream health systems. The absence of
an effective referral system is inconsistent with the right to health.
Coordination—Health systems and the right
to health depend on effective coordination across a range of public and private
stakeholders (including non-governmental organisations) at the national and
international levels. Effective coordination between various sectors and
departments, such as health, environment, water, sanitation, education, food,
shelter, finance, and transport is important for health systems, which also
require coordination within sectors and departments, such as ministries of
health. The need for coordination extends to policy making and delivery of
services.36, 52 Uganda has recently added several
interventions, such as de-worming of children, supplementation with vitamin A,
and health promotion information, to its Child Health Days. Now known as Child
Health Days Plus, these days depend on, and reinforce, improved coordination
between and within sectors and national and international partners, including
civil society.78,
79
International
cooperation—Health
systems have international dimensions, including the control of infectious
diseases, the dissemination of health research, and regulatory initiatives,
such as the International Health Regulations58
and the WHO Framework Convention on Tobacco Control.80
The international dimension of health systems is reflected in countries'
human-rights responsibilities of international assistance and cooperation that
can be traced through the Charter of the UN, the Universal Declaration of Human
Rights, and some more-recent international human-rights declarations and
binding treaties.81,
82 At least, all countries have a human-rights
responsibility to cooperate on transboundary health issues and to do no harm to
their neighbours.83
High-income countries have an additional responsibility to provide appropriate
international assistance and cooperation in health for low-income countries.
High-income countries should especially help others fulfil their core
obligations.36 The Swedish International
Development Cooperation Agency (SIDA), for example, supports several
stakeholders with crucial roles in relation to the right to health in Uganda.
The agency has given funds to various organisations: the Ugandan Government;
WHO for its human-rights work in Uganda; the Uganda Human Rights Commission;
and civil-society organisations, including Straight Talk, which aims to
increase understanding of adolescence, sexuality, and reproductive health.84
For their part, low-income countries have a responsibility to seek appropriate
international assistance and cooperation to help them strengthen their health
systems.85
General
comment 14 confirms that the human-rights responsibility of international
assistance and cooperation in health extends to countries' actions as members
of international organisations.36 Scandinavian countries, for
example, have proposed a trust fund for justice and human rights in the World
Bank.85—87
Legal
obligation—Crucially,
the right to the highest attainable standard of health gives rise to legally
binding obligations. The health system must have, for example, a comprehensive
national health plan; outreach programmes for the disadvantaged; a minimum
package of health-related services and facilities; effective referral systems;
arrangements to ensure the participation of those affected by decision making
in health; respect for cultural difference; and so on. One of the distinctive
contributions of the right to the highest attainable standard of health is that
it reinforces good health practices with legal obligation and accountability.
States are legally obliged to take all appropriate steps to implement the
right-to-health features of health systems. Of course, some governments
implement these features without reference to the right to health. But many
governments do not ensure that these features are in place, and, in these
cases, the right to health has an especially important role.
Monitoring
and accountability—Individuals
and communities should have the opportunity to understand how those with
responsibilities have discharged their duties and provide those with
responsibilities the opportunity to explain what they have done and why.88 Where mistakes have been made,
accountability requires redress. Accountability is not a matter of blame and
punishment but a fair and reasonable process to identify what works, so it can
be repeated, and what does not, so it can be revised.88
Something
as complex and important as health systems needs effective, transparent,
accessible, and independent accountability mechanisms—health commissioners,
national human-rights institutions, democratically elected local health
councils, public hearings, patients' committees, impact assessments, and
judicial proceedings. The media and civil-society organisations also have
crucial roles.88
Accountability
in many health systems is extremely weak. In some countries, the same body
provides and regulates health services, as well as holding those responsible to
account. Accountability can also be little more than a device to check that
health funds were spent as they should have been. Human-rights accountability
is concerned with ensuring that health systems are improving, and the right to
the highest attainable standard of health is being progressively realised, for
all, including disadvantaged individuals, communities, and populations.
In
some countries, although playing an important part, the private health sector
is largely unregulated. The requirement of human-rights accountability extends
to both the public and private health-related sectors89
and to international bodies working on health-related issues.
Accountability
mechanisms are urgently needed for all bodies—public, private, national, and
international—working on health-related issues. The design of appropriate and
independent accountability mechanisms needs creativity and leadership, such as
recently shown by the Uganda Human Rights Commission with the launch of its new
Right to Health Unit in Kampala.90
Scope and
objectives
We
begin to assess the degree to which the health systems of 194 countries include
features arising from the right to the highest attainable standard of health.
From
the start, this project did not aim to give a weighting to indicators nor to
rank countries in an index, although we are aware that ranking can appeal to
politicians and sometimes might enhance monitoring and accountability, leading
to improved health and respect for human rights.91, 92
Ranking in league tables is also problematic with technical difficulties and
problems of interpretation.93
However, indicators and benchmarks are needed to measure the present condition
of a country's health system and to monitor its progress over time. We hope
that this project will be repeated periodically so that the progress of
individual countries, in relation to health systems and the right to health,
can be monitored.
Although
much more work has to be done to help governments identify the minimum package
of health-related services and facilities needed by the right to the highest
attainable standard of health, that vital task is not our aim here. In this
Report, we do not attempt to provide a list of essential services and
facilities needed for a well-functioning health system. Rather, we attempt to
identify several additional, and commonly neglected, features arising from the
right to health and informed by good practices that are required of all health
systems.
Methodology
Development and
selection of indicators
Our
aim was to assess how much the health systems of all countries include some of
the features that arise from the right to health. To meet this aim, we
identified the following objectives: to promote awareness of the complementary
relation between a health system and the right to health; to select a
manageable set of indicators to assess the degree to which a health system
includes some of the right-to-health features; to assess if sufficient
information is available about these features both nationally and
internationally; to increase monitoring and accountability in relation to
health systems and the right to the highest attainable standard of health; to
deepen the understanding of the important role of health data and indicators in
relation to the progressive realisation of the right to health; to consider the
limitations of data for health and human rights in relation to the progressive
realisation of the right to health; to provide a basis to monitor, over time,
health systems and the progressive realisation of the right to the highest
attainable standard of health.
We
developed indicators to reflect right-to-health features of health systems. The
features arise from general comment 14,36 including core obligations, and
reflect many of the themes of the Declaration of Alma-Ata,94
and elements of the WHO building blocks of a health system.75 We also referred to article 24
of the Convention of the Right of the Child,6
general comments 3 and 4 of the Committee on the Rights of the Child,95,
96
and general recommendation 24 of the Committee on the Elimination of the
Discrimination Against Women.97
We also relied on the framework of structure, process, and outcome indicators
on the right to the highest attainable standard of health,98 and the requirement that health
facilities and services should be available, accessible, culturally acceptable,
and of good quality.36
To
ensure that a similar project had not already been done, we reviewed existing
projects (both published and in draft form) relying heavily on indicators, such
as the Human Development Reports,99
the World Health Report 2000 on health systems,52 the WHO and Office of the High
Commissioner of Human Rights (OHCHR) indicators joint project of 2008,100 the UN Millennium Development
Goals,101
the poverty-reduction indicators from OHCHR,102
the WHO essential-medicine indicators,103
and indicators of UNICEF,104
UNAIDS,105
and the World Bank.106,
107
The
development and selection of indicators was a lengthy process with numerous
stages. We selected indicators according to the following criteria: scientific
robustness, usefulness, representativeness, understandability, and importance.91
Data availability was not a determining factor. We also selected indicators
that would be accessible to a broad group of professions, including policy
makers in both health and human rights.
In
an ongoing process over 18 months, we consulted different individuals who
helped in the selection of indicators, including academics (eg, from political
science, law, health, and sociology), UN bodies, national and local
non-governmental organisations and associations, health practitioners, lawyers,
economists, and anthropologists. Individuals were consulted from Africa, Latin
America, Europe, North America, and Asia-Pacific, with balance between sexes.
We also consulted people from indigenous communities. We used purpose sampling
to address specific questions and right-to-health features. We also asked
delegates at two health and human-rights conferences (Italy and Zimbabwe) for
their views, and consulted Maori and non-Maori people in New Zealand. However,
our consultation process could have been better and we suggest that, when our
selection of indicators is revisited, more consultations should take place.
We
used five steps in the process of indicator selection. First, we reviewed the
right-to-health features of health systems and WHO building blocks and, after
numerous consultations, we created a preliminary working model as a way to assist
development and selection of indicators (figure 1). We focused on the wellbeing of individuals,
communities, and populations. We also recognised the importance of
health-related services, facilities, and goods, including underlying
determinants of health, water, sanitation, food, shelter, and education.
Additionally, we identified a selection of features that were of particular
importance to health systems. We revised and refined this preliminary model
because we were aware that it had shortcomings—eg, the model did not clearly
convey that several of the features, such as non-discrimination, are recurrent.
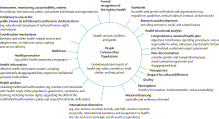
Figure
1 Full-size image (136K)
Right-to-health
features of a health system underpinned by legal obligations based on general
comment 14: preliminary working model
Second,
we looked closely at health-related services and the underlying determinants of
health (middle section of figure 1) in the context of the right-to-health requirements—ie,
that these should be available, accessible, culturally acceptable, and of good
quality. However, of these four requirements, we focused on the first
(availability) and second (accessibility). From the right-to-health
perspective, access is crucial because of its relation with non-discrimination,
equality, and equity. Health care (eg, antenatal, mental-health, cancer care,
and access to medicines), underlying health determinants (eg, drinking water),
and government spending on health care were also taken into account (webtable 1).
Third,
we considered the features shown in the perimeter of figure 1. Formulation of indicators for standards proved
difficult. Formal recognition of the right to health is important but it is
usually confined to a few vague sentences. A more detailed elaboration is
needed by way of legislation, protocols, guidelines, codes of conduct, and others.
We therefore considered formulating indicators that questioned whether
countries had adopted international standards on blood safety and water
quality, but we were unable to identify indicators conforming to our criteria.
We
recognise that planning is only a means to an end. Nonetheless, general comment
14 underlines the importance of planning. An appropriate plan, prepared with a
suitable process, is a vital vehicle for realising the right to health. Thus,
we devoted great attention to the identification of appropriate indicators in
relation to devising a comprehensive national health plan (webtable 2).
We
struggled to identify indicators of participation that conformed to our
criteria. Especially challenging were indicators capturing whether a country
has appropriate institutional mechanisms for participation. Participation
should not be confined to the development of the national health plan; it
should also extend to the national health-workforce strategy, national medicine
policy, implementation measures, accountability, and so on. Furthermore,
participation should not be confined to marginalised groups. However, the right
to health has a special focus on disadvantaged people. But, if marginalised
groups are participating, we can be confident that non-marginalised groups are
too. In the end, we addressed participation in the context of national health
planning.
Indicators
for research and development in health were also challenging. We wanted to
identify indicators that showed whether adequate and appropriate research and
development are being undertaken in a country, but we failed to identify an
indicator that conformed to our criteria, and so this issue is not present in
our final selection.
Fourth,
we aimed to merge the two sets of draft indicators already identified (webtables 1 and 2) and revise them where appropriate. Also, we
wanted to add some new indicators. For example, we were looking for an
indicator that reflected the right-to-health requirement that health-related
services, facilities, and goods should be culturally acceptable. General
comment 14 emphasises that special attention should be paid to indigenous
people and so, prompted by the indicators joint project of WHO and the OHCHR,100, 108
we added a new draft indicator—ie, the proportion of people covered under
indigenous or alternative systems of health care (webtable 3). However, placing indigenous and alternative health
systems in the same indicator was confusing; therefore, this indicator was not
included in our final list. Other indicators approach aspects of cultural
acceptability, such as the indicator about participation of marginalised
groups. Also, the definition of a comprehensive national health plan extends to
the whole population, including indigenous people, and incorporates public and private
sectors, including traditional and indigenous health practices and medicines.
Fifth,
we made a final selection of 72 indicators (panel 4), divided into 15 groups. Some of the groups overlap; for
example, the participation indicator overlaps with the planning indicators. Of
course, many different health workers are crucially important, but some
indicators use doctors and nurses as proxies. After consultations, we created a
new group—additional safeguards—for indicators that did not fit neatly into any
other group. By placing indicators on monitoring, assessment, accountability,
and redress at the end of the list, we are not saying that such issues only
arise at the end of a process. On the contrary, these issues must be seen as
recurrent elements in a continuous process.
Panel
4
Indicators
of right to health
Recognition
of the right to the highest attainable standard of health
- Number of international and regional human-rights
treaties recognising the right to health ratified by the state
- Does the state's constitution, bill of rights, or other
statute recognise the right to health?
Non-discrimination
- Number of treaty-based grounds of discrimination that
the state protects out of: sex; ethnic origin, race, or colour; age;
disability; language; religion; national origin; socioeconomic status,
social status, social origin, or birth; civil status; political status, or
political or other opinion; and property
- Number of non-treaty-based grounds of discrimination
that the state protects out of: health status (eg, HIV/AIDS); people
living in rural areas; and sexual orientation
- General provisions against discrimination
Health
information
- Does the state law protect the right to seek, receive,
and disseminate information?
- Does the state law require registration of births and
deaths?
- Does the state have a civil registration system?
- Does the state disaggregate data in the civil
registration system on grounds of: sex, ethnic origin, rural or urban
residence, socioeconomic status, or age?
- What proportion of births is registered?
- Does the state regularly collect data, throughout the
territory, for the number of maternal deaths?
- Does the state centralise these data for the number of
cases of maternal deaths?
- Does the state make publicly available these data for
the number of cases of maternal deaths?
- Does the state regularly collect data, throughout the
territory, for the number of neonatal deaths?
- Does the state centralise these data for the number of
cases of neonatal deaths?
- Does the state make publicly available these data for
the number of cases of neonatal deaths?
National
health plan
- Does the state have a comprehensive national health
plan encompassing public and private sectors?
- Has the state undertaken a comprehensive national
situational analysis?
- Before adopting its national health plan, did the state
undertake a health impact assessment?
- Before adopting its national health plan, did the state
undertake any impact assessment explicitly including the right to health?
- Does the state's national health plan explicitly
recognise the right to health?
- Does the state's national health plan include explicit
commitment to universal access to health services?
Participation
- Is there a legal requirement for participation with
marginalised groups in the development of the national health plan?
Underlying
determinants of health
- What percentage of the rural and urban population has
access to clean water?
- What are the CO2
emissions per capita?
- Prevalence rate of violence against women
Access
to health services
- Proportion of women with a livebirth in the last 5
years who, during their last pregnancy, were seen at least three times by
a health-care professional, had their blood pressure checked, had a blood
sample taken, and were informed of signs of complications
Medicines
- Is access to essential medicines or technologies, as
part of the fulfilment of the right to health, recognised in the
constitution or national legislation?
- Is there a published national medicines policy?
- Is there a published national list of essential
medicines?
- What is the public per capita expenditure on medicines?
- What is the average availability of selected essential
medicines in public-health facilities?
- What is the average availability of selected essential
medicines in private-health facilities?
- Percentage of 1-year-old children immunised against
measles
- Percentage of 1-year-old children immunised against
diphtheria, tetanus, and pertussis
Health
promotion
- Does state law require comprehensive sexual and
reproductive-health education during the compulsory school years for boys
and girls?
- Proportion of 15—24-year-old boys and girls with
comprehensive HIV and AIDS knowledge
Health
workers
- Does the state have a national health-workforce
strategy?
- Does the state law include provision for adequate
remuneration for doctors?
- Does the state law include provision for adequate
remuneration for nurses?
- Do the state's workforce policies or programmes include
a plan for national self-sufficiency for doctors?
- Do the state's workforce policies or programmes include
a plan for national self-sufficiency for nurses?
- Do the state's workforce policies or programmes provide
incentives to promote stationing in rural areas of doctors?
- Do the state's workforce policies or programmes provide
incentives to promote stationing in rural areas of nurses?
National
financing
- Is the per capita government expenditure on health
greater than the minimum required for a basic effective public-health
system?
- What is the proportion of households with catastrophic
health expenditures?
- Total government spending on health as percentage of
gross domestic product (GDP)
- Total government spending on military expenditure as
percentage of GDP
- Total government spending on debt service as percentage
of GDP
- Proportion of national health budget allocated to
mental health
International
assistance and cooperation
- Does the state's international development policy
explicitly include specific provisions to promote and protect the right to
health?
- Does the state's international development policy
explicitly include specific provisions to support the strengthening of
health systems?
- Proportion of net official development assistance
directed to health sectors
Additional
safeguards
- Does the state law require protection of
confidentiality of personal health data?
- Does the state law require informed consent to
treatment and other health interventions?
- Does the constitution protect freedom of expression?
- Does the constitution protect freedom of association?
- Does the state have a patients' rights charter?
- Is the patients' rights charter available in all
official languages?
Awareness
raising about the right to the highest attainable standard of health
- Does the state have a national human-rights institution
with a programme of budgeted activities to raise awareness of the right to
health among the public?
- Does the state have a national human-rights institution
with a programme of budgeted activities to raise awareness of the right to
health among doctors?
- Does the state have a national human-rights institution
with a programme of budgeted activities to raise awareness of the right to
health among nurses?
- Are human rights a compulsory part of the national
curriculum for the training of doctors?
- Are human rights a compulsory part of the national
curriculum for the training of nurses?
Monitoring,
assessment, accountability, and redress
- Infant mortality rate
- Mortality rate of children younger than 5 years
- Maternal mortality ratio
- Life expectancy
- Does the state have a national human-rights institution
with a mandate that includes the right to health?
- Number of judicial decisions, nationally, that
considered the right to health during 2000—05
- Does the state have a national human-rights institution
with a mandate to monitor international assistance and cooperation?
- In the past report submitted by the state to the UN in
relation to the International Covenant on Economic, Social, and Cultural
Rights, was there a detailed account of the international assistance and
cooperation in health that the state is providing?
As
prioritised by general comment 14, several indicators focus on maternal and
child health. Women and children are among those groups that are often
marginalised. In the past 2—3 years, maternal mortality has increasingly been
recognised as a human-rights issue.109—111
We
prepared explanatory notes for each indicator, along the lines of the
meta-sheets used in the recent indicators joint project of WHO and the OHCHR.100
Explanatory notes for every indicator include: definitions, rationale, method
of computation, data source, periodicity, comments, and limitations (webappendix 1). Each data source was assessed for its quality and
any potential bias was noted.
To
reduce the number of indicators, disaggregation of all appropriate indicators
on all relevant grounds was not required, although we acknowledge that such
data should be available. Several of the selected indicators, however, address
discrimination, including the indicator on civil registration requiring
disaggregation on five priority grounds: sex, ethnic origin, rural or urban
residence, socioeconomic group, and age. We identified these priority grounds
of disaggregation through a process of consultation between lawyers and health
workers, including representatives from the British Medical Association, WHO, and
academic institutions. Ideally, all appropriate data should be disaggregated,
at least, by these five priority grounds. The civil registration system should
be one of the most comprehensive data-collection systems in a country, and
therefore this indicator was chosen as the proxy measure.
We
did not identify indicators of all right-to-health features conforming to our
selection criteria (eg, indicators related to coordination and research and
development). Although several indicators exist addressing different dimensions
of access, such as indicators 24 (access to clean water), 27 (antenatal care),
and 46 (catastrophic health expenditure), we accept that issues of access
demand more attention.
External review
After
selection of draft indicators, we sent them and explanatory notes to 40
experts, who had not previously been part of this project, for their comments
and review. 22 experts responded, including lawyers, human-rights
professionals, clinicians, public-health practitioners, academics, and policy makers.
We recognise the advantages of random sampling, but constraints of time and
resources prevented this approach. However, expert comments were very
constructive in deciding and devising the final version of our list of
indicators.
Data collection
To fulfil
the project's objectives, we needed to consider data availability at the global
level and, in relation to five countries, at the national level as well.52, 112 For a few indicators, only the global
perspective was necessary (eg, the number of international and regional
treaties recognising the right to health ratified by a country). If information
was not present about a particular indicator, it was marked as not available in
the Table 1, Table 2. If an indicator was not applicable to a
particular country, it was marked as such. The time period for data collection
was from August, 2007, to August, 2008, with the intention of obtaining data
for the same indicators at about the same time.
We
initially selected six countries for national data collection because one of
us, PH (then the UN special rapporteur on the right to the highest attainable
standard of health) had recently been to them on mission and prepared formal UN
reports on each before this project began. Only five could commit to data
collection in the allotted time: Sweden, Mozambique, Romania, Peru, and
Ecuador. Although not globally representative, these high-income,
middle-income, and low-income countries provided a range of different political
background, history, geographical location, and cultural contexts. Countries
such as China, Bangladesh, USA, and India would have been interesting to study,
but they fell outside our selection criteria. In each of the five countries
selected, we chose data collectors who, at the relevant time, were independent
from the government (although they might have collaborated closely with the
government) and had a good knowledge of the country, of health and human
rights, and preferably of the right to health.
For
every indicator, the information obtained was the response to the indicator,
the source of the data, and the date of last update and of access (if from an
internet source). Relevant comments to explain the answer were documented, in
addition to exact legal provisions for indicators related to the law and exact
quotes for indicators related to plans or policies. In addition to table 1 on global data (194 countries) and table 2 on national data (five countries), webtables 4 and 5 include extended tables with sources, comments,
and other information. The International Committee of Medical Journal Editors
Uniform Requirements was used as the basis for the referencing system.113
For internet sources, the date of access and of last update was of particular
importance to document. The working currency for all monetary data was US
dollars at the exchange rate at the time of data collection.
We
clearly defined terms used for indicators that were strictly adhered to during
data collection; although this rigidity might have led to reduced data
availability. All relevant definitions can be found in the explanatory notes
online (webappendix 1).
Data
were accepted in any of the official UN languages: Arabic, Chinese, English,
French, Russian, and Spanish, with translations into English done by the team
where necessary. National data were received in English, Spanish, or Swedish,
and translated where necessary.
Primary
data were not collected; therefore, formal ethical approval was not necessary
for this research project. Only secondary data were used on both global and
national levels. All the information was in the public domain, defined to be
any document that is in print and should be easily accessible, such as in a
library or on the web.
To
ease collection of global data, we created the so-called one-click rule, which
defines that the limits of the search for data should only be no more than one
mouse click away from the global source. For example, if, while navigating
through the WHO website, a link to a national website was found, then the link
would be opened. If the required information was accessible on that webpage,
then it would be judged as globally processed data and therefore acceptable.
If, however, there was need to follow more than one link, open tabs, or for any
navigation other than scrolling up and down, the information was not judged as
globally available. This rule only applied to links to webpages outside the
global source, with no limitations imposed on navigation within the global
source. We decided that this rule was needed to provide a practical limit to
what could otherwise become an eternal internet search, but still allowing
adequate and useful data collection.
We
generated a list of global websites (webappendix 2). If any data were unavailable in any of these
websites, we did a more detailed search. We identified suitable search terms
where necessary; these are documented in the explanatory notes that accompany
each indicator (webappendix 1).
Sometimes,
the presence of a right-to-health feature was not apparent at the global level,
which could be interpreted as the data were not existing. However, in these
situations we reported that the information was not available, which meant that
it might exist and be documented elsewhere. For example, if there was no
mention of a national health-workforce strategy in the information available at
the global level, then the data were listed as unavailable for that country.
However, if the information stated that there was no health-workforce strategy,
then that was recorded with a ‘no’.
Methods
for data collection nationally were slightly different and defined as
accessible information in the public domain. These data were needed to be
publicly available and therefore included information available on the
internet, published reports, or information publicly available on request. We
requested documentation of the source. Data that were only available to
selected groups or information acquired through interviews were not allowed.
National teams of data collectors could decide how best to search for the
information as long as it fulfilled the methodological requirements. National
teams searched relevant websites and published documents unrestricted by the
one-click rule. However, they were restricted to national sources and could not
access global databases, such as UN sources. We relied on the same explanatory
notes (webappendix 1) to ensure that definitions and criteria were
consistent with the global data and the same referencing guidelines were
applied. We are aware of some limitations of the methods.
For
some indicators, a year was included from which data were collected (identified
in webappendix 1). The project started in 2007 and data were often
not yet available for 2007, or even 2006, and therefore data from 2005 were
often the most up-to-date (further information is available in webtables 4 and 5 and explanatory notes in the webappendix 1). Furthermore, the indicator relating to judicial
decisions was restricted to cases within a 5-year period (2000—05) because we
thought that this was a manageable recent timeframe.
Several
indicators we selected are commonly used (eg, indicator 68 on life expectancy),
and information is available in published material about their usefulness,
validity, and limitations.
Because
of the many differing lists of states worldwide, we opted to use a list of 194
countries generated from the WHO member-state list of 200052
and those countries listed by the UN Development Programme,112
acknowledging that other lists may differ. Several indicators were only
applicable to donor states, and the list of states to be considered for these
indicators was compiled from Organisation for Economic Co-operation and
Development (OECD) members114
and the International Development Association of the World Bank list of donors
from March, 2008115
(webpanel). However, the indicator may be related to an event that
happened before a state was a donor, such as the past report in relation to the
International Covenant on Economic, Social, and Cultural Rights.
Key findings
We
discuss some of the key findings and results arising from the data collected
for the 72 indicators, giving special attention to three of our objectives. Do
countries' health systems have the relevant right-to-health features? Are the
relevant data available at the global level? Do the data provide a basis to
monitor, over time, health systems and the progressive realisation of the right
to the highest attainable standard of health.
We
did not try to find directional relations between variables, such as treaty
ratification and health outcomes. Several indicators in our list illustrate
that, no matter how sophisticated they are, indicators never provide a complete
picture and they need to be supplemented with qualitative information. Table 1 summarises the global data from 194 countries and table 2 the national data from five countries. All data are
available in webtables 4 and 5.
Recognition of the
right to health
Recognition
of the right to the highest attainable standard of physical and mental health
is a right-to-health feature of a health system. Although recognition can have
various forms, we focused on international (indicator 1) and national
(indicator 2) recognition (panel 4). Figure 2
shows the number of countries that have ratified three international
human-rights treaties that include the right to health. The step after
ratification of treaties is the recognition of the right to health in the
national constitution or other statute, but more than two-thirds of countries
do not have this recognition. Only 56 countries that have ratified the
International Covenant on Economic, Social, and Cultural Rights include the
right to health in their constitution or other statute. International
recognition of the right to health (indicator 1) is substantially more
widespread than national recognition (indicator 2), probably because
international accountability is weaker than national accountability.
Number
of countries that have ratified treaties that include the right to health
CRC=Convention
on the Rights of the Child. ICERD=International Convention on the Elimination
of Racial Discrimination. ICESCR=International Covenant on Economic, Social,
and Cultural Rights.
Although
legal recognition of the right to the highest attainable standard of health can
mean commitment towards the realisation of the right to health, this does not
capture the actual process or success of implementation. Other indicators
attempt to do this and are discussed later. Legal recognition is important
because it can increase accountability of stakeholders with responsibilities
to, and within, a health system.
Although
eight indicators explicitly mention the right to health, different countries
use different terminology for this human right. Some countries use terminology
that does not match our wording, and negative results were recorded in these
cases (webappendix 1). Online documents were sometimes translations of
original documents, introducing another possible reason for different
terminology.
Non-discrimination
We
aimed to record aspects of non-discrimination, equality, and equity—key
right-to-health features of health systems. Indicator 3, for example, lists 11
treaty-based grounds of discrimination, and indicator 4 lists three
non-treaty-based grounds of discrimination (panel 4).
The treaty-based ground of discrimination most commonly protected by law was
ethnic origin (122 countries), whereas the least-protected was age (13
countries; figure 3). However, 95 countries protect only five or less
treaty-based grounds of discrimination, and none protects all 11.
We
addressed non-discrimination asking whether data in the civil registration
system were disaggregated on the five priority grounds of sex, ethnic origin,
rural or urban status, socioeconomic group, and age (indicator 9). None of the
five countries studied nationally disaggregate these data by ethnic origin, and
therefore they cannot show any inequity between ethnic groups. Disaggregation
of data on the basis of ethnic origin is a controversial issue and, although
such information can be used in a positive way, it can also be used in a
negative way (eg, to reinforce stigmatisation). Therefore, article 8 of the EU
Data Directive prohibits the “processing of personal data revealing racial or
ethnic origin”, but with important exemptions related to data processed by
health professionals.116
For
non-treaty-based grounds of discrimination, protection was even less widespread
than for treaty-based grounds (figure 3).
For example, according to our approach, only three countries (Fiji, South
Africa, and Ecuador) protected against discrimination on the ground of sexual
orientation.
People
with mental illnesses are frequently neglected and discriminated against, and
this might lead to inadequate financial provision for mental health.44
Therefore, we took into account the proportion of the national health budget
allocated to mental health (indicator 50). Of 98 countries for which data were
available, almost half allocated 2% or less of their national budget to mental
health. Sweden and Ecuador did not allocate a specific budget for mental
health. The team gathering data in Sweden remarked that this is “partly a
consequence of the objective to not stigmatise the group” (webtable 4). We do not agree that a specific budget allocation for
mental health could stigmatise those with mental-health problems or that it is
inconsistent with the integration of mental-health care across health systems.
By contrast, the absence of a specific budget allocation might maintain the
marginalisation and neglect experienced by many people with mental
disabilities.
Later,
we consider the indicator on access to clean water (indicator 24).
Disaggregated on the basis of urban or rural residence, this indicator confirms
the disadvantage of rural dwellers in most countries.
Health information
Because
of its crucial importance in relation to both the right to health and the WHO
building blocks, health information is prominent in our profile of indicators
(indicators 6—16). We focused on maternal and neonatal deaths, and the civil
registration system. We questioned whether countries obtained data for the
number of maternal deaths throughout their territory. On the basis of global
data and our approach, 69 countries obtained, centralised, and made publicly
available these data; whereas 88 countries did not. Data for the remaining 37
countries were unavailable at the global level, including those for Ecuador and
Peru. Compared with data for maternal deaths, data for neonatal deaths were
available at a global level for even fewer countries. Nationally, data were
gathered, centralised, and made publicly available by Ecuador, Romania, and
Sweden (panel 5);
however, Mozambique did not do this for maternal deaths (they only include
those deaths occurring in institutions) and Peru did not for neonatal deaths.
Overall, on the basis of our approach, 88 countries do not seem to have in
place an adequate health information system for maternal deaths, suggesting
that their health systems are seriously deficient in terms of both the right to
health and relevant WHO building blocks. Also, despite their importance, global
data for maternal and neonatal deaths are inadequate.
Panel
5
Civil
registration in Sweden
The
law on national civil registration in Sweden provides registration of births to
registered parents. When a child is born in Sweden to non-registered parents,
such as undocumented immigrants, the child will not be registered. Information
about number of births to non-registered parents is unreliable. The picture is
complicated by the fear of many non-registered people of Swedish authorities.
As
with equity, human rights have a particular concern for marginalised
individuals, groups, and populations. Several indicators in the profile take
into account disadvantaged groups, such as indicators on discrimination
(indicators 3—5), participation with marginalised groups (indicator 23), and
whether or not the patients' rights charter is available in all official
languages (indicator 59). Disadvantage cannot be monitored without data that
are disaggregated on key grounds.117
We questioned whether a country disaggregates data from the civil registration
system on the priority grounds of sex, ethnic origin, rural or urban residence,
socioeconomic group, and age (indicator 9). On the basis of our approach, no
global data were available for any country. However, research in the five
selected countries showed that national data were available.
All
five countries disaggregated on two of the five grounds (sex and age); only one
country (Romania) disaggregated on four of the five grounds, and none disaggregated
on the ground of ethnic origin, which makes the design of appropriate
interventions that address ethnic disadvantage very difficult for policy
makers. Lack of disaggregated data also makes it difficult to hold countries
accountable for accessibility of their health systems. From the right-to-health
perspective, this shortcoming is important.
Overall,
our data confirmed that disaggregated information, which is crucial for right
to health, even when available nationally, is not always made available globally.
National health
plan
According
to general comment 14, the adoption of a national public-health strategy and
plan of action is a core obligation.36
An
essential precondition for the development of a comprehensive national-health
plan is a national health situational analysis (indicator 18). Global data
showed that 57 countries had done health situational analyses, although all
were done as a part of the WHO country cooperation strategy development
process.118
However, global data were not available for the other 137 countries. Data were
more readily available nationally than they were globally. For example,
although global data are not available for Romania, national data confirmed
that they have not done a health situational analysis. Indicator 18 does not
capture whether the analysis was used to develop the national health plan or
the quality of the analysis, as shown in panel 6
for Mozambique. Nonetheless, the existence of a health situational analysis is
an important precondition for a national health plan and a step in the right
direction. Our research confirmed that, despite the importance of health
situational analyses, global data collection neglects this right-to-health
feature.
Panel
6
National
health situational analysis in Mozambique
Before
the development of its national health sector strategic plan, Mozambique
undertook a comprehensive national health situational analysis. This analysis
identified health problems of disaggregated population groups, such as
children, and the feminisation of HIV. It also showed the effect of gender in
the fight against HIV, and the need to improve human resources for health at
all levels. It identified possible interventions, such as high vaccination
coverage, to control diseases in children younger than 5 years and the
improvement of campaigns on behaviour change. The analysis emphasised the need
to reinforce support systems and focused attention on the importance of
monitoring and assessing health programmes and services. However, close
examination also showed issues with the quality of the information gathered and
data analysis.
Assessments
of health and human-rights effects are also needed, together with a
comprehensive national health plan. There is a growing trend to undertake
health impact assessments before a health initiative is finalised, adopted, and
implemented.75 We asked whether countries
undertook either a health impact assessment (indicator 19) or any impact
assessment that included the right to health (indicator 20) before adopting their
national health plan. Of course, indicators have limitations; for example, even
with an impact assessment, any negative findings might be ignored and the plan
implemented without revision. No global data were available with our approach
for any country regarding either indicator. Nationally, none of the five
countries did a health impact assessment before adopting their national health
plans. We confirmed that, despite the importance of such assessments, global
data collection ignores this important right-to-health feature of a health
system.
We
asked whether a country has a comprehensive national health plan encompassing
public and private sectors (indicator 17). Our explanatory notes (webappendix 1) identified the essential criteria of a plan, such
as clear objectives, timeframes, indicators, benchmarks, and reporting
procedures. For 181 countries, we were unable to gather global data with our
approach, and 13 countries do not have a comprehensive national health plan—ie,
their health systems lack this important right-to-health feature. However, the
indicators for national health plans highlighted limitations of the internet as
a resource. Dates of last updates are commonly unavailable, and therefore
information might be out of date. Although we made every effort to gather data
as completely and accurately as possible, with such an extensive database there
might be inaccuracies. Nonetheless, despite the importance of a comprehensive
national health plan, global data collection seems to neglect this important
right-to-health feature of a health system.
More-detailed
national data were available for the comprehensive national health-plan
indicators, showing that Mozambique, Romania, and Sweden have comprehensive
national health plans, whereas global data were not available. At the time of
data collection, Peru was preparing a national health plan but it did not
include all the features of a comprehensive health plan (panel 7).
Panel
7
Participation
in Peru's health councils
Representatives
of Peru's ForoSalud (a nationwide civil-society network) obtained support from
the minister of health and the national health council for their proposal to
change the composition of national, regional, and provincial health councils.
The existing composition included nine representatives of health providers and
only one of health-service users. The new proposal promotes a more bottom-up
approach to participation, including discussion of new health policies, with a
plan to repeat the participatory process in 2 years and 6 months. The aim is to
promote accountability of government officers for both the achievements and
shortcomings of health policy.
We
asked whether the national health plan includes an explicit commitment to
universal access to health services, defined as access to primary, secondary,
and tertiary physical and mental care (indicator 22). We regarded a commitment
to basic or essential care as inadequate. A low-income country might not be in
a position to deliver universal access to health services, but a comprehensive
national health plan should include a commitment to reach this aim.36 Such a commitment is the minimum
expected from all countries, whatever their stage of economic development. A
developing country's commitment to universal access gives an important message
to health workers, the public, and donors. When a country cannot provide
universal access, it must have fair, transparent, rational, evidence-informed
processes (eg, protocols and guidelines) in place to ensure that reasonable
decisions are made when determining who has access to health-related facilities
and services, and on which terms.
On
the basis of global data and our approach, national health plans of 15
countries (Antigua and Barbuda, Bahrain, Botswana, Chile, North Korea,
Dominican Republic, Honduras, Libya, Mauritius, Mozambique, Peru, Seychelles,
Timor-Leste, Uruguay, and Yemen) include an explicit commitment to universal
access to health services, whereas plans of 14 countries (Afghanistan, Argentina,
Bangladesh, Bolivia, Costa Rica, Croatia, Egypt, El Salvador, Lesotho, Malawi,
Nepal, Papua New Guinea, Romania, and Tanzania) do not. However, global data
are not available for 165 countries. Again, our research suggests that global
data collection neglects information that is important for the right to health.
We
also asked whether the country's national health plan explicitly recognises the
right to the highest attainable standard of health (indicator 21). Explicit
human-rights language can be useful for policy makers and empower disadvantaged
individuals, communities, and populations. On the basis of global data and our
approach, two national health plans secured a yes, four secured a no, and data
were not available for the remaining 188 countries. >From the
right-to-health perspective, global data collection is seriously deficient.
Participation and
its preconditions
Despite
the importance of participation to both health systems and the right to health,
no global data, with our approach, were available for any country for indicator
23. At the national level, of the five countries, none legally required
participation of marginalised groups in the development of their national
health plan. This finding suggests that participation is not receiving the attention
it demands; although some countries have made provision for the participation
of citizens, without specifying marginalised groups. WHO building blocks of a
health system give insufficient attention to the role of participation.30
Active
and informed participation depends on several factors. Preconditions for
meaningful participation include having access to information (eg, access to
the health budget), being free to speak openly without intimidation (eg,
publicly criticise a local health council), being free to organise with no
restriction (eg, establish an independent medical association or patients'
group), and meeting without impediment (eg, hold a public meeting). These are
also necessary safeguards for meaningful implementation of other
right-to-health features, such as health promotion. Some of these preconditions
are present in our selection of indicators. For example, the law in 121
countries does not protect the right to information (indicator 6); the law in
41 countries does not protect freedom of expression (indicator 56); and in nine
countries the law does not protect the right of association (indicator 57). In these
countries, preconditions for meaningful participation or effective health
promotion do not exist.
However,
reality is worse than these data suggest. Although the law might protect
information, expression, association, and assembly, in some countries a wide
gap exists between law and implementation. This does not mean that the law is
without value. Rather, it recognises that the law is a tool, and therefore its
usefulness depends on circumstances, including the creativity of those who use
it. We addressed this more-practical, non-legal dimension of preconditions,
with special attention to access to information. Global data showed that 88
countries do not gather, centralise, and make publicly available the number of
maternal deaths (indicators 11—13). Without such vital health information,
meaningful participation can be an empty promise.
Underlying
determinants of health
We
included indicators on the underlying determinants of health (eg, access to
clean water, CO2 emissions per person, and
violence against women [indicators 24—26]). The relation between diarrhoea (and
other health conditions) and access to clean water is well known.119 Thus, we asked what percentage
of the population has access to clean water—defined as at least 20 L per person
per day from a source within 1 km of the user's dwelling (indicator 24).119,
120
This indicator raised important definitional issues that were briefly
considered in the explanatory notes (webappendix 1).
Only
54 countries had more than 90% of their rural population with access to clean
water and only 115 countries had more than 90% of their urban population with
access to clean water (panel 8). Rural dwellers are disadvantaged in most countries for
clean water access (figure 4).
We used the joint monitoring programme as the source for these data because it
shows where the original data come from, as opposed to some other sources that
do not or only use estimates. We identified the method and year of data
collection in the extended data tables (webtables 4 and 5) to emphasise that data were obtained from
various sources, including national surveys and the joint monitoring programme
estimates, and that some data were from 1990.121 Comparison of data between
countries is therefore difficult, which is why we did not rank countries.
Romania has less than 20% of its rural population with access to water, and the
difference in access to water between rural and urban populations is striking
(16% vs 91%).121
Data available at the national level were more recent and showed that, by 2005,
the gap had narrowed a little but was still extreme (34% vs 92%).122
Panel
8
Access
to clean water in Mozambique
In
Mozambique, poor access to clean water is responsible for serious illnesses and
leads to frequent outbreaks of cholera. Access to clean water has improved in
rural communities through close coordination with the ministry of public works
and with support from various donors. Recent data confirmed this improvement
and showed a higher rate of access to clean water in rural (48·5%) than in
urban (40%) areas. However, urbanisation has taken place across Mozambique in
recent years, leading to a large influx of people into cities and, therefore,
in provision of the necessary infrastructure to ensure access to water in urban
areas.
We
aimed to provide a basis to monitor, over time, the progressive realisation of
the right to the highest attainable standard of health. The indicator for
access to clean water is especially useful for monitoring a country's
progressive realisation. Romania's data for access to clean water in rural and
urban areas should be revisited in a few years. If there is an acceptable
measure of improvement, the government will be able to argue that, in
accordance with its international human-rights obligations, it is progressively
realising this aspect of the right to health. But if access to clean water
remains the same or becomes worse, the government will have the burden of
proving that all has been done to try to improve access to clean water. If the
government cannot show that all that is possible has been done, it will be in
breach of its international human-rights obligations. This example illustrates
the importance of independent, transparent, and accessible accountability
mechanisms that can decide whether any improvement that might have occurred is
acceptable in the circumstances. If the government has fallen short of its
responsibilities, accountability mechanisms should consider appropriate
redress, which ranges from guarantees of non-repetition to compensation.88
Definitional
issues restricted data availability for violence against women (indicator 26),
the indicator of which has suitable data only for eight countries (Bangladesh,
Brazil, Ethiopia, Japan, Namibia, Peru, Tanzania, and Thailand from the WHO
multicountry study on women's health and domestic violence against women).123
Although a lot of data exist for this subject, definitions vary for violence,
domestic violence, violence against women, and even women (as defined by age),
making it challenging to find comparable data.
Access to health
services
We
addressed different dimensions of access, such as those of antenatal care
(indicator 27), access to clean water (indicator 24), and catastrophic health
expenditure (indicator 46), but more work is needed to identify appropriate
indicators that measure access. We asked what is the proportion of women with a
livebirth in the last 5 years who, for their last pregnancy, were seen at least
three times by a health-care professional, had their blood pressure checked,
had a blood sample taken, and were informed of signs of complications
(indicator 27). This indicator uses antenatal care as a proxy for primary care
and coverage to represent access. We obtained data for this composite indicator
from the world health survey with information available for 51 countries, 19 of
which are categorised as low-income and 22 as middle-income countries.124,
125
The
world health survey includes women aged 18 years and older, and therefore data
exclude those under 18 years who also need antenatal care and might be a group
with reduced access to services. Those women whose pregnancy did not result in
a livebirth are not included and they may be less likely to have received
adequate antenatal care. Furthermore, women could be reluctant to acknowledge a
livebirth when the child only survived a few minutes, and could falsely refer
to this as a stillbirth. These are a few examples of limitations associated
with this indicator showing an overestimation of the percentage of women who
received care. Even with these overestimations, less than 50% of women had
comprehensive antenatal care in 33 of 51 countries (figure 5).
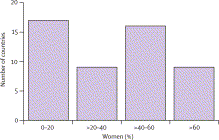
Figure
5 Full-size image (18K)
Percentage
of women by number of countries who had comprehensive antenatal examinations
during their last pregnancy
N=51
countries.
Similar
to the indicator on access to clean water, the antenatal-care indicator can be
used to measure the progressive realisation of an important aspect of the right
to health. For example, according to global data and our approach, only 12% of
women in India have comprehensive care. India's data should be revisited in the
future to assess whether the government is progressively realising this
important aspect of the right to health.
Health workers
One
of the WHO building blocks of a health system, health workers have a key role
in the implementation of the right to the highest attainable standard of health
(panel 9).
Because of their importance, 11 indicators address issues directly related to
them (indicators 38—44 and 61—64). On the basis of global data and our
approach, we found that 21 countries have a national health-workforce strategy
and 12 do not, whereas for 161 countries data were not available. Using doctors
and nurses as proxies, we looked at remuneration, national self-sufficiency,
incentives to promote stationing in rural areas, awareness raising, and
human-rights training. Of the 11 indicators that relate to health workforce,
eight do not have global data available (including four in the
awareness-raising group).
Panel
9
Health
workers in Romania
Romania
has one of the lowest densities of health personnel in Europe in relation to
doctors, nurses, dentists, and pharmacists. Furthermore, there is an imbalance
between regions of the country. In rural areas, there are 98 communities
(villages) without any doctor, and the situation is comparable for nurses and
other health workers. In a third of Romania, more than 30% of medical
specialties are not available. The accession of Romania to the EU aggravated
the situation with 10% of doctors seeking work outside Romania, according to a
recent survey of the Romanian College of Physicians. This situation increases
already existing inequities between rural and urban populations. Payment types
currently compensate rural better than urban clinicians for the same type of
services. However, the existing additional benefit payment programme has not
met its goal of providing a sufficient health workforce in the underserved
areas. These data suggest that a comprehensive approach is needed to tackle
more than the financial dimension of the issue. The ministry of health has
proposed additional incentives to try to increase and stabilise the number of
health workers in rural areas.
International
assistance and cooperation
Human-rights
responsibility has several components, including the duty of high-income
countries to provide, and low-income countries to seek, international
assistance and cooperation. We set five indicators for human-rights
responsibility in health (indicators 51—53, 71, and 72). All five indicators
focus on the responsibility of donors rather than on the responsibility of
recipient countries.
We
asked whether donors' international development policies explicitly include
specific provisions to promote and protect the right to health in recipient
countries (indicator 51), and whether these policies explicitly include
provisions to support the strengthening of health systems (indicator 52). No
global data based on our approach were available for any donor in relation to
either indicator. Nationally, however, some data were available. National data
in Sweden confirmed that the country's international development policies
explicitly include specific provisions on the right to health, whereas national
data in Romania led to the opposite conclusion. Also, national data in Sweden
and Romania confirmed that both countries' international development policies
explicitly include provisions to support the strengthening of health systems.
We
also asked about the percentage of net official development assistance directed
to health sectors (indicator 53): Italy (17%), Ireland (15%), Netherlands
(14%), and Denmark (11%) seemed to be far ahead, whereas Japan, Greece, and
Luxembourg (all 1%) seemed to be a long way behind (panel 10).
Panel
10
Official
development assistance for G8 member countries (global level data)
Italy—17·48%
USA—7·26%
Canada—6·43%
France—3·74%
Germany—2·93%
UK—2·37%
Japan—1·13%
Russia
Federation—Not available
However,
in recent years some donors have moved away from the provision of funds for
specific sectors towards general budget support. Because of the Paris
Declaration on Aid Effectiveness, this trend is likely to accelerate.82
For this reason, a brief narrative should accompany this indicator to explain
each country's approach to overseas development assistance and health, for
example, to signal if the donor is moving away from sectoral support towards
general budget support. Donors' support should be in line with the growing
international recognition that, if the health-related Millennium Development
Goals are to be achieved, health systems must be strengthened.
Our
research suggests that, for indicators 51 and 52, the relevant global data,
based on our approach, are globally unavailable. We also noted that the
relevant national data were available for Sweden and Romania. Data gathered for
indicator 53 provided a basis to monitor, over time, donors' progressive
realisation of their human-rights responsibility of international assistance
and cooperation in health.
Monitoring, assessment,
accountability, and redress
Eight
indicators were grouped together under monitoring and accountability
(indicators 65—72); however, several others might properly be regarded as
monitoring and accountability indicators, such as those on impact assessments
(indicators 19 and 20).88
Monitoring
and accountability depend on the availability of reliable and relevant data.
Without indicators, benchmarks, and data, it is not possible to monitor the
progressive realisation of the right to health. Several traditional health
outcome measures have a key role. A worsening health outcome, such as maternal
mortality, does not necessarily mean that a country is failing its
right-to-health responsibilities. However, it obliges a country to explain to
an appropriate accountability body why the situation is deteriorating.
We
took into account three mortality measures: infant mortality (indicator 65),
mortality of children younger than 5 years (indicator 66), and maternal
mortality ratio (indicator 67), together with life expectancy (indicator 68).
Of these, the one with the least global data available was maternal mortality
ratio. Data exist for 169 countries with a range from 1 (Ireland) to 2100
(Sierra Leone) per 100 000 livebirths (mean 331).126 This range is astounding
because most deaths are preventable and a high ratio shows that the health
system is failing.
As
with other indicators already discussed, such as antenatal care and access to
water, indicators 65—69 can be used as a basis to monitor, over time, aspects
of the progressive realisation of the right to health.
111
countries have national human-rights institutions, many of which make a
substantial contribution to the promotion and protection of human rights.
Although independent, these institutions are non-judicial and designed to be
more accessible, flexible, and informal than courts.127
One of their functions is to monitor and hold governments accountable. We asked
whether a country has a national human-rights institution with a mandate that
includes the right to the highest attainable standard of health (indicator 69).
Is the institution empowered to monitor public and private health and hold
accountable those with right-to-health responsibilities? No global data for
this indicator were available with our approach for any country. Data were
available, however, nationally. Of the five countries, three (Ecuador, Peru,
and Romania) have national human-rights institutions, and the mandate of each
extends to the right to health. With leadership and resources, these
institutions could contribute greatly to constructive accountability for the
right to health (panel 11).31
Panel
11
Monitoring
and accountability in Peru
Over
the past year, Cooperative for Assistance and Relief Everywhere (CARE)-Peru and
Physicians for Human Rights have supported the development of citizen and
civil-society accountability mechanisms at both district and local levels. An
example is in the Piura and Puno regions, where Quechua and Aymara women
community leaders have been linked to regional offices of the human-rights
ombudsman to monitor women's health rights, particularly their right to good
quality, appropriate maternal health services. Rural women's leaders have also
been empowered by a joint agreement between ForoSalud and the human-rights
ombudsman office in Puno. Partnerships have been mutually enriched, with women
leaders feeling better positioned to demand information and changes in health
services.
We
also asked whether national human-rights institutions have a mandate to monitor
donors' human-rights responsibility of international assistance and cooperation
(indicator 71). However, no global data based on our approach were available
for any donor for this indicator. National data showed that, although three of
the five countries have national human-rights institutions, none of these
institutions has a mandate to monitor international assistance and cooperation
in health.
Countries
that have ratified international human-rights treaties have an obligation to
report on their activities related to that treaty usually within 2 years.5
A committee of independent human-rights experts publicly considers the report
and may ask country's representatives challenging questions about the
government's record, publishing its concerns and recommendations. A few years
later the process is repeated and the experts' committee asks the country to
explain what has been done in relation to the earlier recommendations. Under the
International Covenant on Economic, Social, and Cultural Rights, donor
countries should report on their human-rights responsibilities of international
assistance and cooperation in health. Therefore, we took into account country's
reporting on international assistance and cooperation in health to the UN
Committee on Economic, Social, and Cultural Rights (indicator 72). We showed
that only three donor countries (Belgium, Canada, and Japan) reported
adequately on this crucial issue.
Low-income
countries have the perception that high-income countries escape accountability
when failing to fulfil their international pledges and commitments that are
important to developing countries.28
Data seem to confirm that this perception is right. Our national data suggest
that the mandates of national human-right institutions do not extend to holding
donors to account for their human-rights responsibility of international
assistance and cooperation. Also, most donor countries are not being held
accountable by a key UN human-rights treaty body for their responsibility of
international assistance and cooperation in health. We conclude that donor
countries are subject to only feeble independent, institutional scrutiny for
their international responsibilities.
In
63 countries, the constitution, bill of rights, or other statute recognise the
right to health. Legal recognition serves many purposes. In several countries,
for example, it made the authorities accountable before the courts, leading to
tangible improvements in health services.55, 56 We, therefore, enquired about the number of
judicial decisions that took into account the right to health in 2000—05
(indicator 70). However, it is possible that the decision may not promote and
protect this fundamental human right. Nonetheless, even in this case, at least
the country is held accountable for the right to health, having to explain
itself before an independent accountability body.
Global
data disclosed, on the basis of our approach, only five countries (Canada,
Nigeria, Peru, South Africa, and Venezuela) with judicial decisions conforming
to this indicator. The combined number of judicial decisions is less than ten.
This is striking because in recent years numerous national courts have decided
right-to-health cases, and yet our data show that they are not globally
available in accordance with our approach.55, 56
Here,
we looked at some of the right-to-health features and their data, and conclude
that health systems in numerous countries do not have the features required by
the right to health. Also, there are insufficient data currently available,
especially at the global level, to assess these indicators in relation to many
countries. Figure 6
shows the unavailability of global data in relation to a selection of 25
indicators for which it is clear that, in many cases, international bodies are
not collecting the appropriate right-to-health data. An overarching conclusion
is that those at the international and national levels with responsibilities
for health systems seem to be giving inadequate attention to the
right-to-health analysis and some of the features required by the right to
highest attainable standard of health..
Opportunities and
challenges
On a
country-by-country basis, table 1 summarises the degree to which health systems of countries
include some features that arise from the right to health in relation to 72
indicators. Table 2 summarises national data for the same indicators in
relation to five countries. When considering the performance of an individual
country, the country's stage of economic development (what human-rights
treaties refer to as the countries resource availability) is important.
Some
of our findings are positive: for example, we record high rates of vaccination
with measles-containing vaccine (MCV) and diphtheria, tetanus, pertussis (DTP3)
vaccine (indicators 34 and 35). General comment 14 places a high priority on
immunisation programmes.36 Although such programmes can
occur as vertical interventions, whenever possible they should strengthen
health systems. Weak health systems impede high immunisation coverage128 and the GAVI Alliance and Fund
Boards recently increased funding for health system strengthening to US$800
million.128
We recorded good practices for the implementation of right-to-health features
of health systems, such as Mozambique's effective coordination between
different stakeholders to improve access to safe water in rural communities (panel 8).
Also, Sweden has recently introduced the legal requirement for inclusion of
human rights in the training curriculum of health workers, reflective of
indicators 63 and 64.129
Countries
that have not put in place some of the key features of a health system—eg, a
comprehensive national health plan (indicator 17), a published national list of
essential medicines (indicator 30), a national health workforce strategy
(indicator 38), or government expenditure on health per person above the
minimum required for a basic effective public health system (indicator 45)—are
in breach of their right-to-health responsibilities whatever their stage of
economic development.
We
provide a basis on which to monitor health systems and the progressive
realisation of the right to health. A suitably improved version of this project
repeated in a few years' time will give an indication of whether countries have
progressively realised the right to health. Take, for example, a high-income
country in which prevalence of violence against women has increased (indicator
26); access to health services (indicator 27) has worsened; immunisation of
1-year-old children against measles (indicator 34) has decreased; total
government spending on health as a percentage of GDP (indicator 47) has
lessened; and life expectancy has fallen. In such a case, progressive
realisation of the right to health has not been achieved. Unless the government
has a rational, objective explanation for the worsening situation (eg, a
natural disaster), this country would be in breach of its right-to-health
responsibilities.
We
have emphasised the limitations of indicators generally and some of our
indicators specifically. Moreover, as we have seen, there are some
inconsistencies between global data (table 1)
and national data (table 2).
So the data must be used with caution.
In
this Report, we concentrate on recognition of the right to health;
non-discrimination; health information; national health plan; participation;
underlying determinants of health; access to health services; health workers;
international assistance and cooperation; and monitoring, assessment,
accountability, and redress. We do not discuss some important right-to-health
features and their data, such as finance and medicines, because space
restrictions compelled us to be selective.
Limitations
to indicator selection and data collection do not contradict the profile of
indicators or the findings, but should be considered when analysing the
results. We hope that the profile of indicators will prompt discussion and that
subsequent revisions will make indicators more robust.
This
project relies on secondary data published by others, and any limitations of
the primary data affect our dataset. Because of resource constraints,
triangulation of data collection was not included in the methods, except when
checking for an unexpected result. The number of indicators is large, but we
did not want to compromise too much. When the project is repeated, we suggest
an assessment of concordance of the data. Although one of the objectives of
this project was to assist with monitoring progressive realisation of the right
to health, some of the indicators, such as maternal mortality ratio, are not
sensitive to change over short periods. Additionally, so-called yes or no
indicators do not lend themselves to measurement of gradual change over time,
although many are complemented by a commentary (webtables 4 and 5) to explain the result that could indicate
improvement with time.
For
this project, restrictions on collection of worldwide data were needed.
However, the one-click rule introduced elements of inconsistency in the data
collection. Some regions tended to have more information available within the
limits of the one-click confines than others—for example, lists of WHO member
states each link to some documents about that country. For some regions,
detailed information was available on global websites, whereas, for others,
global websites were structured in such a way that the one-click rule allowed
only an index page for the region, not the actual information, to be reached.
Also, there was a risk of further discrepancy in data available for developed
countries and those available for developing countries. This discrepancy might
arise because international organisations assist developing more than developed
countries in data collection or analysis, and these data are subsequently more
readily available worldwide.
Our
research shows that insufficient data are available, especially at the global
level, in relation to right-to-health features. From the perspective of health
systems and the right to health, UN bodies and other international stakeholders
are not collecting appropriate data. International and national institutions
with responsibilities for health systems seem to be giving inadequate attention
to the right-to-health analysis and some of the features needed for the right
to the highest attainable standard of health. Here we focus on other areas of
concern and make recommendations. We do not attempt to discuss all our concerns
and recommendations but focus on those arising from some key areas. Taking into
account both the right-to-health analysis outlined in this report and the data
collected, we make additional recommendations in panel 12.
Panel
12
Recommendations
We
recommend WHO and the Office of the High Commissioner for Human Rights
- adopt a stewardship role in the collection and
collation of data for right-to-health features of a health system
- lead the process to establish universal definitions for
commonly used terms and standardised units of measurement regarding the
right-to-health features of a health system
- maintain and regularly update a global data repository
on the right-to-health features of a health system
- lead the process to establish, where appropriate,
international benchmarks to assess country performance regarding the
right-to-health features of health systems
- ensure that the Global Health Workforce Alliance
gathers data relevant to the right to health, such as for human rights
training for health workers
We
recommend other UN specialised agencies and bodies
- coordinate with WHO, national governments,
civil-society organisations, and other international, regional, and
national stakeholders to ensure coherence in global monitoring with
respect to the right-to-health features of a health system
- provide technical assistance to national governments to
facilitate data collection on the right-to-health features of a health
system
- record descriptive and numerical data
- cooperate with WHO, national governments, civil-society
organisations, and other relevant stakeholders to establish universal
definitions for common terms and standardised units of measurement of
right-to-health features of health systems
- ensure that the activities of the UN specialised agency
or other body are aligned with the comprehensive national health plan
We
recommend national governments
- explicitly recognise the right to health, and
right-to-health features, such as access to essential medicines, in the
national constitution or statute
- ensure explicit recognition of the right to health in
the comprehensive national health plan
- ensure sufficient expenditure on medicines to provide,
as a minimum, equitable access to essential medicines
- collect data on marginalised groups to inform the
planning and development of the health system
- do health and human-rights impact assessments before
finalising the comprehensive national health plan
- in partnership with WHO, UN specialised agencies, civil
society, and others, collect and regularly update information on
right-to-health features of health systems
- disaggregate data on at least the five priority
prohibited grounds of discrimination—sex, age, ethnicity, socioeconomic
status, and rural or urban residence
- regularly submit information updates about the
right-to-health features of health systems to the global data repository
maintained by WHO/OHCHR
- cooperate with the WHO, UN bodies, and others in
establishing national and international benchmarks to monitor the
right-to-health features of health systems
- ensure registration of births and deaths within a civil
registration system
- establish national human-rights institutions with a
mandate that includes the right-to-health and budgeted programme of
activities for raising awareness about the right to health
- ensure the mandate of the national human-rights
institution includes monitoring and accountability with respect to
international assistance and cooperation in health
- include compulsory human-rights and right-to-health
training for health workers, judges, and lawyers
- submit timely, full reports to the UN Committee on
Economic, Social, and Cultural Rights and other relevant UN treaty bodies
We
recommend national and international civil society
- participates in health system planning and monitoring
- advocates that right to health is properly incorporated
in health system planning
- advocates the inclusion of marginalised groups in
health decision making
- advocates that the mandates of national human-rights
institutions include the right-to-health and budgeted programme of
activities for raising awareness of right-to-health
- disseminate information about key judicial decisions
about the right to health
- ensure that the activities of the civil society
organisation are in alignment with the comprehensive national health plans
We
recommend research institutions
- provide assistance to national governments to do health
and human-rights impact assessments
- do or commission research on the right-to-health
features of health systems;
- actively promote knowledge sharing among academics on
the right-to-health and right-to-health features of health systems
- collaborate with national governments, WHO, UN bodies,
civil-society organisations, and others to promote a greater understanding
of the right to health and right-to-health features of a health system
We
recommend donors
- recognise the importance of strengthening health
systems in international assistance strategies
- allocate greater funding for health in low-income and
middle-income countries
- ensure donor accountability for international
assistance and cooperation in health in both donor and recipient countries
- align international assistance and cooperation
strategies with the comprehensive national health plans of recipient
countries
Recognition of the
right to health
Recognition
of the right to health in international treaties, national constitutions, and
other statutes gives rise to a legal obligation for countries to ensure that
their health systems have certain features, as discussed, and also that the
performance and quality of health systems do not regress or stagnate but
improve over time. However, most countries (121 of the 184 for which data are
available) do not recognise the right to health in their national constitutions
or other statute, although every country has ratified at least one
international treaty that recognises the right to health. Recognition of the
right to health has not only generated judicial decisions that have improved
the delivery of health-related services,55
it has also led to non-judicial mechanisms of accountability, such as the Right
to Health Unit established by the Uganda Human Rights Commission,90
and led to enhanced health policy and practice. For example, the Department of
Health in the United Kingdom recently commissioned an assessment of the
effectiveness of implementing a human-rights based approach in health and
social care.130
Focusing on five pilot projects, the assessment concluded that such an approach
had a noticeable effect on the treatment and care of health-service users, and
that it is one way of achieving good practice. Thus, we recommend that
countries ratify treaties that encompass the right to health, explicitly
recognise this human right in their national constitutions or other statute,
and integrate the right to health into their national health plans.36
Health information
Health
information is the life-blood of effective, accessible health systems and the
right to health. Information enables individuals and communities to promote
their own health and allows governments to formulate evidence-based health plans.
Monitoring, accountability, and participation depend upon access to
information. Without reliable disaggregated data, whether health systems are
delivering access to services and facilities without discrimination is
impossible to know. However, our research suggested that health information
systems in many countries are seriously deficient in several ways.
Health
information systems include a range of data sources, such as censuses,
household surveys, vital registration systems, and other health-facility data
sources.131
Ideally, systems should not duplicate but complement each other, providing
accurate information making best use of limited resources.132 Data for maternal and neonatal
deaths, for example, should be included within the vital registration system,
but the data then need to be specifically extracted, a position supported by
the WHO Maternal Mortality Report in 2005.126
Of 194 countries, 122 have a civil registration system; however, many of these
are incomplete, with fewer than 90% of events registered. Accurate recording of
cause of death according to international standards is important,133
and the statistics generated should then form a part of the situational
analysis that contributes to health-system planning. We recommend that all
countries should legally require registration of births, deaths, and cause of
death according to international standards (using the international
classification of disease).134
The
USAID-supported Demographic Health Surveys, the Multiple Indicator Cluster
Survey programme developed by UNICEF, and other surveys provide much
information. Data provided by these surveys were used as sources for many
indicators in this profile, and for some indicators, such as those considering
access to water and vaccination coverage (see extended data in webtables 4 and 5) the survey type and year were recorded along
with the score. Although surveys fill an important role, they are not the best
long-term solution to collection of routine data if not done regularly and they
should be included in a civil registration system that is permanent,
continuous, compulsory, and universal.132
At the very least, a system is needed to record reliable information on birth
and death registration in all regions. Such a system would have implications
for several human rights. Without birth registration, many entitlements may be
denied throughout life, such as access to health care, education, international
travel, and the right to own property. However, data for the percentage of
births registered in rural and urban areas are only available for 78 countries.
Furthermore, only 69 countries regularly collect, centralise, and make publicly
available data throughout the territory for numbers of maternal deaths. We
recommend, at a minimum, continuous registration of births and deaths in all
areas within a vital registration system.
Descriptive
information is needed to understand the issues behind quantitative data;
however, we often found a shortage of this information. In this project, all
indicators have been reduced to a number or to yes or no answers, but the
accompanying data and commentaries (webtables 4 and 5 and webappendix 1) are crucial to understanding
our findings. Some issues are difficult to accurately capture with purely
quantitative data, and we encourage greater emphasis on a complementary brief
narrative in some cases.135
As
part of their human-rights responsibility of international assistance and
cooperation in health, donors (webpanel)
should accelerate their coordinated efforts to provide training and technical
assistance for sustainable data collection and processing and to make data
available worldwide. Additionally, donors should facilitate the establishment
of national health information systems, including a comprehensive civil
registration system in all countries, with clear mechanisms for relaying this
information to a globally accessible data repository. WHO and the UN Office of
the High Commissioner for Human Rights should have a leadership role in
establishing and maintaining a global system for collection and collation of
up-to-date information from different countries and UN bodies on
right-to-health features of health systems.
Disaggregation
Policy
makers and health practitioners need accurate information about marginalised
groups as many are at risk of worse health,136
because, in many cases, of problems in accessing health-related services. From
the human-rights perspective, the goal is to disaggregate data in relation to
as many of the internationally prohibited grounds of discrimination as possible
(indicators 3 and 4), although some data cannot be disaggregated. The
collection of disaggregated data remains an enormous challenge for many
countries and, because of limited capacity, reliable disaggregated data are
often unavailable. The contextual natures of vulnerability and discrimination
further hamper collection of relevant data: a group might be especially
vulnerable in one context but not in another. We had difficulty identifying
indicators that captured vulnerability and marginalisation, probably because of
their contextual nature. We recommend five priority grounds—sex, age, ethnic
origin, rural or urban residence, and socioeconomic group—for disaggregation as
a minimum.98
These ground are similar to those identified by the Health Metrics Network.59
Some
health issues demand disaggregation on particular grounds; for example, in the
context of sexual and reproductive health, disaggregation on the basis of sex
and age are crucial. Of the 21 countries with information about the proportion
of men and women with comprehensive knowledge of HIV/AIDS, men fared better
than did women in 16, suggesting that different strategies for education of
women are required. The Guidelines on Construction of Core Indicators in
relation to monitoring the Declaration of Commitment on HIV/AIDS note that an
important lesson from the UNAIDS Global Progress Report of 2003 was that
without disaggregated data monitoring of access, equity, and change over time
is difficult.137
The guidelines acknowledge that this disaggregation requires effort, but point
out that such data are commonly collected at the subnational level but
subsequently lost when passed to the national level. Another recommendation
therefore is that coordinated efforts are made to collate and present reliable
data at the national and global levels broken down on the basis of the five
priority grounds.
Coordination
of data
Because
the right to health involves policies and practices that lie beyond the health
sector, effective coordination is needed between different sectors (including
health, transport, environment, and education) and different health services.
General comment 14 recognised coordination as a right-to-health feature of
health systems.36 Data collection is one example
of where coordination is needed—as happens with global maternal mortality data.
UNICEF, WHO, UNFPA, and the World Bank periodically assess maternal-mortality
data.138
As a result of joint assessment the data on maternal mortality are the same at
WHO and UNICEF. However, life expectancy data differ between the two sources;
for example, WHO reports a life expectancy of 61 years in Namibia, UNICEF
reports 52 years. The cause of this large discrepancy is unclear. We recommend
coordination and collaboration between countries, regional stakeholders, UN
bodies, and others to establish a global repository for health data with
up-to-date and consistent reporting.
For
some indicators more information is available worldwide for low-income than for
high-income countries, such as the data on DTP3 and MCV vaccination.139
However, high-income countries have the resources to collect and process the
relevant data, which should be logged in a global repository.
Standardisation
When
developing the indicators and collecting data, one major difficulty was the
lack of universal definitions for many commonly used and important terms, such
as clear definitions for rural and urban. Disaggregation of data on these
grounds was therefore difficult; in practice, individual data collectors decide
whether a location is rural or urban.140
Similarly, violence against women does not have a standard definition.141
Specific criteria and definitions should be created, although they might not
capture every nuance of the relevant issue, to allow consistency of data
collection and comparison over time.
Standard
definitions are needed to create national and international benchmarks against
which to measure a country's progress. General comment 14 anticipates that
countries and the UN Committee on Economic, Social, and Cultural Rights will
agree key indicators and then identify appropriate benchmarks or targets to be
achieved by the country over the next few years in relation to the selected
indicators.36
Agreed indicators and country-specific benchmarks are needed to measure
progressive realisation and hold governments to account. Sometimes benchmarks
are agreed internationally for all countries, or a group of countries—for
example, all donors should devote 0·7% of their gross national income to
overseas development assistance, and all African leaders have pledged to
allocate 15% of their annual budgets to health.142
Whether benchmarks are set nationally or internationally, standard definitions
are important. For example, CO2 emissions are
recorded in various ways, which makes benchmarking difficult.143
Although indicators and benchmarks are vital if we wish to measure progressive
realisation and hold countries to account, their usefulness depends on widely
agreed definitions.
Standard
formatting for data collection would be especially helpful in low-income and
middle-income countries that have to collect similar information in different
formats to fulfil the demands of different donors and international bodies.
We
warmly welcome the Health Metrics Network, a global partnership of UN bodies,
donors and others aiming to improve health information at country, regional,
and global levels.59
The network hopes that by 2011 its detailed framework and standards for country
health information systems will be the universally accepted standard for all
developing countries and global agencies. The network comments on the
inappropriate use of data collection methods (eg, surveys used to record adult
mortality) and advocates the disaggregation of health-status data. We recommend
that the network encourages the collection of data outlined in this report,
which is needed to measure the right-to-health features of a health system.
Access
to information is part of the right to health. However, in addition,
information is protected by national and international codes of civil and
political rights.144
Many of these codes provide stronger accountability mechanisms than are
available to the right to health. We recommend that human-rights workers in the
domain of civil and political rights use their expertise to improve access to
health information, following the example of the London-based civil society
organisation Article 19.
Comprehensive
national health plans
Within
the confines of our methods, no data currently are available at the global
level to show that any country has a comprehensive national health plan,
whereas 13 countries have data available on the WHO website indicating that
they do not have a comprehensive national health plan. We recommend adoption of
a universal definition of a comprehensive national health plan. Countries
should develop comprehensive national health plans consistent with defined
criteria, including budget allocation for all proposed activities. Information
about all such plans should be available both nationally and internationally.
Monitoring and assessment of these plans both nationally and at the global
level are also needed to ensure compliance with agreed criteria. Any gaps
identified should be systematically addressed; for example, if a national
health plan does not encompass the private sector then this shortcoming needs
to be identified and remedial action taken.
Appropriate
national and international human-rights bodies should monitor whether or not a
country has a comprehensive national health plan conforming to the agreed
criteria. For example, a national human-rights institution should check whether
or not the government has an appropriate national plan. Most national
human-rights institutions report annually to the legislature and the status of
a national plan could be publicly reported this way. Also, appropriate
international committees of human-rights experts, such as the UN Committee on
Economic, Social, and Cultural Rights, should routinely ask countries appearing
before the committee about their comprehensive national health plans. The UN
Human Rights Council has recently established a new procedure that all
countries must follow. Known as the universal periodic review, a comprehensive
national health plan is so important that the council should routinely ask all
countries about the status of their plan.145
Monitoring,
assessment, accountability, and redress
We
recommend that much closer attention be devoted to establishing accessible,
transparent, and effective mechanisms for monitoring and accountability of
health systems and the right to health. Analysis of the data collected in this
project reveals weak mechanisms at international and national levels. Without
indicators and reliable data, neither the condition of health systems nor the
progressive realisation of the right to health is possible. Accountability,
however, is much more than monitoring. Organisations and individuals with
right-to-health responsibilities must be held to account in relation to the
fulfilment of their duties, with a view to identifying successes and
difficulties—what Freedman31
calls constructive accountability. In this way, accountability strengthens
health systems.
As
explored by Potts,88 there are many different
mechanisms of monitoring and accountability for the right to health—social,
political, administrative, quasijudicial, and judicial—each with a crucial
role. Our indicator 69 tried to address quasijudicial accountability by asking if
countries have national human-rights institutions with mandates that include
the right to health. However, there was no globally available data for this
indicator revealing either a shortfall in the data available or in the mandates
themselves. We recommend that national human-rights institutions include the
right to health in their mandates and budgets for programmes.146
In close collaboration with the health sector, these institutions could provide
human-rights training for health workers, raise public awareness of
right-to-health entitlements and processes, work with public officials to
integrate the right to health into policies, help to prepare right-to-health
protocols and guidelines for health workers, monitor right-to-health features
(eg, comprehensive national health plans and international assistance and
cooperation in health), and undertake independent public inquiries into
particular right-to-health issues, hold those responsible to account, and make
recommendations. Australia's Human Rights and Equal Opportunity Commission has
made health inquiries on several occasions, for example, in its Social Justice
Report 2005 that applies human rights to indigenous health policy.147
With the recent change of government in Canberra, this important report is now
shaping health policy and practice. National human-rights institutions should
forge strategic partnerships with the media, health workers, patients' groups,
judges, lawyers, academics, and others.
Mechanisms
of social accountability include public hearings and social audits. The
People's Health Movement in India has set up the People's Rural Health Watch to
conduct independent health monitoring in seven states in northern India. This
initiative supplements the community monitoring that is part of the National
Rural Health Mission launched by the government in 2005.88 In some situations, Médecins
Sans Frontières, after listening to patients to understand why a situation is
occurring, will draw attention to the issues, problems, and responsibilities.148
One
example of administrative accountability is addressed in the indicators for
impact assessment (a process through which the potential effects of a policy,
programme, or plan on the health of the population is assessed). However, data
for the national level show that none of the five countries had made a health
impact assessment or any impact assessment including the right to health before
the implementation of their national health plan. We recommend that countries
make such assessments before adopting their national health plan; there should
at least be an impact assessment in relation to key elements of a plan. Such
assessments can be crucial to progressive realisation of the right to health.75
Effective
monitoring and accountability depends on numerous factors, including the
recognition of the right to health as a legally enforceable right. Where the
rule of law is respected, it helps to be able to say to the relevant minister,
local health council, or hospital director that a particular health initiative
is not only ethically appropriate and good practice but is also required under
binding national and international human-rights law. Accountability is not
judicial accountability. As discussed, judicial accountability is one narrow,
limited form; moreover, it is accountability of last resort. Judges and lawyers
must be willing to learn about, and apply in a balanced manner, such
right-to-health concepts as progressive realisation, resource availability,
core obligations, and disadvantage; they must be willing to listen to health
experts and those using health-related services. Information about key judicial
decisions for realisation of the right to health should be widely accessible.
Also, countries must report regularly on regional and international treaties
that they have ratified.
Redress
is another important component of accountability.88
It comes in many forms, such as full and public disclosure of the truth,
apology, acknowledgment of responsibility, a change in policy, law reform,
rehabilitation (eg, the provision of health-related services), and
compensation.
Finally,
careful attention must be given to the human-rights accountability of
international bodies, as well as the private sector. The Human Rights
Guidelines of Pharmaceutical Companies in relation to Access to Medicines can
deepen the accountability of the pharmaceutical sector.149
Additional research
This
project highlights the need for more research on the right to health. For
example, what are the core obligations signalled in paragraph 43 of general
comment 14? Research is needed on the application of the right to health to the
six WHO building blocks of a health system and within both public and private
sectors. More attention should be devoted to right-to-health features of health
systems: for example, what are appropriate mechanisms of monitoring and
accountability? More research is needed on the most appropriate indicators for
assessing the degree to which health systems include these right-to-health
features. We had particular difficulty identifying appropriate indicators in
relation to access (including access for marginal groups), respect for cultural
difference, quality, participation, referral systems, standards (ie, provisions
that elaborate in more detail upon the general right-to-health formulations
found in treaties, constitutions, and statutes), coordination (ie, the need for
effective coordination across a range of public and private stakeholders, at
the national and international levels, both within and between health-related
sectors), and monitoring and accountability. We recommend that particular
thought be given to identifying appropriate indicators for these issues.
Echoing Gruskin and colleagues,39
we also recognise the need to build evidence of the effects of the application
of the right to health on health systems.
Conclusion
Over
18 months of research, our interdisciplinary project has depended upon the
insights of experts in both health and human rights. UN bodies,
non-governmental organisations, policy makers, academics, and others have made
indispensable contributions. We strongly recommend that all those sharing the
common ground between health and human rights deepen their dialogue,
cooperation, and collaboration. Our findings have implications for professions
and institutions at all levels and in both public and private sectors. For
example, health ministries and national human-rights institutions need to meet
and talk, and UN organisations must routinely discuss health and human-rights
issues. For example, WHO, UNFPA, and the World Bank must engage with the UN
Human Rights Council, Office of the High Commissioner for Human Rights, and
human-rights-treaty bodies. All these organisations—and many others—have the
common aim of strengthening health systems.
Countries
have a legal obligation to progressively realise the right to the highest
attainable standard of health and therefore to improve their health systems
progressively. Indicators and benchmarks are needed to measure present
conditions of health systems and to monitor them over time. Indicators selected
in this profile and methods of data collection have limitations, but the
findings have generated several recommendations. We are drawn to the conclusion
that those with responsibilities for health systems are giving inadequate
attention to the right-to-health analysis. Our main, overarching recommendation
is that all those with health-related responsibilities explicitly consider the
right-to-health analysis and integrate this human right into their policies and
practices, with a view to strengthening health systems. We hope that this
project will be repeated periodically so that the progress of individual
countries will be monitored. No doubt improvements will be introduced to the
methodology and profile of indicators before the exercise is repeated in a few
years' time.
This
project rests on the conviction that an equitable health system is a core
social institution, no less than a fair court system or democratic political
system. Because of its importance, a health system is reinforced and protected
by the right to the highest attainable standard of health and other human rights.
Health systems should have certain right-to-health features identified in this
report. These features are legally binding requirements, not optional extras.
Governments must be held to account to ensure that health systems have, in
practice, the features required by international human-rights law.
Contributors
As
project director, GB contributed to the drafting of all sections and
explanatory notes and collected global data. PH contributed to the drafting of
all sections. GB and PH prepared figure 1.
RK contributed to the drafting of the introductory, key findings, and
opportunities and challenges sections and explanatory notes and collected
global data. CJ-S and BMF contributed to the drafting of the methodology
section and the explanatory notes and collected global data. CR contributed to
the drafting of the methodology, key findings, the opportunities and challenges
sections and explanatory notes and collected global data. DP contributed by
advising on statistical analysis and developing several and reviewing all of
the figures in the key findings section. DA and MAP collected national data on
Ecuador. AF and DT collected national data on Peru and drafted some panels. MM
collected national data on Mozambique and drafted some panels. CV and DF
collected national data on Romania and drafted some panels. DAP, CJ-S, AF, and
DT, write in a personal capacity and the views expressed are not those of their
affiliations.
Conflict
of interest statement
We
declare that we have no conflict of interest.
Acknowledgments
We
are extremely grateful to the following individuals who have provided us with
assistance: Idris A Bawa, Alexandra Cameron, Edelisa D Carandang, Judith Bueno
de Mesquita, Aditi Das, Louise Finer, Malebakeng Forere, Jane Godsland, Sofia
Gruskin, Hans Hogerzeil, Dragana Korljan, Richard Laing, Rhona MacDonald,
Gillian MacNaughton, Maxwell Madzikanga, Paulo Marchi, Sophie Mathewson, Martin
McKee, Ellen Nolte, Uju A Okereke, Lisa Oldring, Ching-Ling Pang, Genevieve
Paul, Justina Pinkeviciute, Helen Potts, Anna Protano—Briggs, Mike Rowson,
Julian Sheather, Christine Tapp, Daniel Tarantola, Michael Wilks. This report was
researched with support from the Ford Foundation and Joseph Rowntree Charitable
Trust. However, the content of the report is the sole responsibility of the
authors and cannot be taken to reflect the views of either the foundation or
trust.
References
1
UN. Universal
Declaration of Human Rights. G. A. Res. 217A (III), UN GAOR, Res. 71, UN Doc.
A/810. New
York: United Nations, 1948.
2
BrownlieI. Basic
documents of international law. Oxford: Oxford University Press, 2006.
3
MarksS. Health and
human rights: Basic international documents. Cambridge: François-Xavier Bagnoud Center for Health
and Human Rights, Harvard School of Public Health, 2006.
4
UN. International
Covenant on Economic, Social and Cultural Rights (ICESCR). New York: United
Nations, 1966.
5
SepúlvedaM. The nature of
the obligations under the International Covenant on Economic, Social and
Cultural Rights. Utrecht: Intersentia, 2003.
6
UN. Convention
on the Rights of the Child (CRC). New York: United Nations, 1989.
7
UN. International
Convention on the Elimination of all Forms of Racial Discrimination. New York: United
Nations, 1996.
8
KinneyEClarkB. Provisions for health and health care in the
constitutions of the countries of the world. Cornell Int Law J 2004; 37: 285-355. PubMed
9
WHO. Constitution of the World Health Organisation. http://www.who.int/gb/bd/PDF/bd46/ebd46_p2.pdf. (accessed Sept 21, 2008).
10
WHO. Declaration of Alma-Ata, international conference on
primary health care, Alma-Ata, USSR. http://www.searo.who.int/LinkFiles/Health_Systems_declaration_almaata.pdf.
(accessed Sept 21, 2008).
11
WHO. Ottawa charter for health promotion, first
international conference on health promotion Ottawa. http://www.who.int/hpr/NPH/docs/ottawa_charter_hp.pdf.
(accessed Sept 21, 2008).
12
WHO. The Bangkok charter for health promotion in a
globalized world. http://www.who.int/healthpromotion/conferences/6gchp/hpr_050829_%20BCHP.pdf.
(accessed Sept 21, 2008).
13
Ministry of Health, Government of Uganda.
Review of the HSSPII in relation to human rights
and gender as part of third-term review for the health sector, second draft
June 2008. Kampala: Ministry of Health, 2008.
14
WHO. Human
rights, health and poverty reduction strategies.
Geneva: World Health Organization, 2005.
15
Constitutional Court, Tutela decision T-760/2008,
Judge: Manuel Jose Cepeda, Second Reviewing Chamber. http://www.corteconstitucional.gov.co/. (accessed Sept 21, 2008).
16
In: Gauri V, Brinks DM, eds. Courting social
justice: judicial enforcement of social and economic rights in the developing
world. Cambridge:
Cambridge University Press, 2008.
17
In: Ghai Y, Cottrell J, eds. Economic, social
and cultural rights in practice: the role of judges in implementing economic,
social and cultural rights. London: Interights, 2004.
18
Inter-American Commission on Human Rights.
Access to justice as a guarantee of economic,
social and cultural rights: a review of the standards adopted by the
Inter-American Commission on Human Rights. Washington: Inter-American Commission on Human Rights, 2007.
19
In: Baderin MA, McCorquodale R, eds. Economic, social
and cultural rights in action. Oxford: Oxford University Press, 2006.
20
Ely YaminAParra VeraO. The role of courts in defining health policy: the case
of the Colombian constitutional court. Harvard Law School Human Rights Program
Working Paper. http://www.law.harvard.edu/programs/hrp/documents/Yamin_Parra_working_paper.pdf.
(accessed Sept 21, 2008).
21
AsherJ. The right to
health: a resource manual for NGOs. London: Commonwealth Medical Trust, 2004.
22
AsherJHammDSheatherJ. The right to
health: a toolkit for health professionals. London: British Medical Association/Commonwealth
Medical Trust, 2007.
23
Physicians for Human Rights. The right to health and health workforce planning: a
guide for government officials, non-governmental organisations, health workers
and development partners. Cambridge: Physicians for Human Rights, 2008.
24
People's Health Movement. The
assessment of the right to health and health care at the country level. http://www.phmovement.org/files/RTH_assmt_tool.pdf.
25
HuntP. Report of the
UN Special Rapporteur on the right to the highest attainable standard of health
to the Commission on Human Rights, UN Doc E/CN.4/2004/49. Geneva: United
Nations, 2004.
26
HuntP. Report of the
UN Special Rapporteur on the right to the highest attainable standard of health
to the United Nations General Assembly UN Doc A/61/338. New York: United
Nations, 2006.
27
HuntP. Report of the
UN Special Rapporteur on the right to the highest attainable standard of health
to the Commission on Human Rights, UN Doc. E/CN.4/2005/51. Geneva: United
Nations, 2005.
28
HuntP. Report of the
UN Special Rapporteur on the right to the highest attainable standard of health
to the United Nations General Assembly UN Doc A/59/422. New York: United
Nations, 2004.
29
HuntP. Report of the
UN Special Rapporteur on the right to the highest attainable standard of health
to the United Nations General Assembly UN Doc A/62/214. New York: United
Nations, 2007.
30
WHO. Everybody's
business: strengthening health systems to improve health outcomes: WHO's
framework for action. Geneva: World Health Organization, 2007.
31
FreedmanL. Achieving the MDGs: health systems as core social
institutions. Development 2005; 48: 19-24. CrossRef | PubMed
32
WeissbrodtD. The right to a
fair trial under the Universal Declaration of Human Rights and the
International Covenant on Civil and Political Rights. The Hague: Martinus
Nijhoff, 2001.
33
International Covenant on Civil and Political
Rights (ICCPR). New York: United Nations, 1996.
34
Zimmerman and Steiner v Switzerland, European Court of Human Rights. A.66
(1983) 6 EHRR 17.
35
HuntP. Report of the
UN Special Rapporteur on the right to the highest attainable standard of health
to the Human Rights Council, UN Doc. A/HRC/4/28.
Geneva: United Nations, 2007.
36
Committee on Economic, Social and Cultural
Rights. The right to the highest attainable standard of health:
11/08/2000. E/C.12/2000/4, CESCR General Comment 14. Twenty-second session
Geneva, 25 April—12 May 2000 Agenda item 3. http://www.unhchr.ch/tbs/doc.nsf/(symbol)/E.C.12.2000.4.En.
(accessed Sept 21, 2008).
37
HuntPBackmanG. Health systems and the right to the highest attainable
standard of health. Health Hum Rights 2008; 10: 81-92. PubMed
38
HuntP. The human right to the highest attainable standard of
health: new opportunities and challenges. Trans
R Soc Trop Med Hyg 2006; 100: 603-607. CrossRef | PubMed
39
GruskinSMillsETarantolaD. History, principles, and practice of health and human
rights. Lancet 2007; 370: 449-455. Summary | Full
Text | PDF(109KB) | CrossRef | PubMed
40
In: Mann J, Gruskin S, Grodin M, Annas G, eds. Health and human
rights: a reader. New York: Routledge, 1999.
41
In: Gruskin S, Grodin M, Annas G, Marks S, eds. Perspectives on
health and human rights. New York: Routledge, 2005.
43
HuntP. The health and human rights movement: progress and
obstacles. J Law Med 2008; 15: 714-724. PubMed
44
HuntPMesquitaJ. Mental disabilities and the human right to the highest
attainable standard of health. Hum Rights
Q 2006; 28: 332-356. PubMed
45
WHO. WHO
Report 2001: Mental health: new understanding, new hope. Geneva: World Health
Organization, 2001.
46
HortonR. What does a national health service mean in the 21st
century?. Lancet 2008; 371: 2213-2218. Full
Text | PDF(109KB) | CrossRef | PubMed
47
International Harm Reduction Association.
Global harm reduction report. London: International
Harm Reduction Association, 2008.
48
HuntP. Report of the
Special Rapporteur on the right to the highest attainable standard of health to
the Human Rights Council, UN Doc A/HRC/4/28/Add.2. Geneva: United
Nations, 2007.
50
Amnesty International. Peru: poor and excluded women—denial of right to
maternal and child health. London: Amnesty International, 2006.
51
Ministerio de Salud. Norma técnica para la atención del parto vertical con
adecuacion intercultural. Lima, Peru: Ministerio de Salud, 2005.
52
WHO. World
Health Report 2000, health systems: improving performance. Geneva: World Health
Organization, 2000.
53
WHO. People
at the centre of health care: harmonising mind and body, peoples and systems. Geneva: World Health
Organization, 2007.
54
TarimoE. Towards a
healthy district. Organizing and managing district health systems based on
primary health care. Geneva: World Health Organization, 1991.
55
SinghAJGovenderMMillsE. Do human rights matter to health?. Lancet 2007; 370: 521-527. Summary | Full
Text | PDF(84KB) | CrossRef | PubMed
56
HogerzeilHVSamsonMVidal CasanovasJRahmaniL. Access to essential medicines as part of the fulfilment
of the right to health—is it enforceable through the courts?. Lancet 2006; 368: 305-311. Summary | Full
Text | PDF(91KB) | CrossRef | PubMed
57
WHO. Who guidelines for drinking water quality. http://www.who.int/water_sanitation_health/dwq/guidelines/en/index.html.
(accessed Sept 21, 2008).
58
WHO. International
health regulations (2005). Geneva: WHO, 2008.
59
WHO. Framework
and standards for country health information systems. Geneva: WHO, 2008.
60
Sphere Project. Humanitarian charter and minimum standards in disaster
response. Geneva:
Sphere Project, 2004.
61
Potts H. Participation and the right to the highest attainable standard of
health. Essex: Human Rights Centre, University of Essex, forthcoming.
62
ManandharDSOsrinDShresthaBP. Effect of a
participatory intervention with women's groups on birth outcomes in Nepal:
cluster-randomised controlled trial. Lancet 2004; 364: 970-979. Summary | Full
Text | PDF(465KB) | CrossRef | PubMed
63
Medicines Transparency Alliance. Website.
http://www.medicinestransparency.org. (accessed Nov 4, 2008).
64
Open Society Institute. Mediating Romani health: policy and programme
opportunities. New York: Open Society Institute, 2005.
65
BravemanPGruskinS. Defining equito in health. J Epidemiol Community Health 2003; 57: 254-258. CrossRef | PubMed
66
Hoffmann v South African Airways. Constitutional
Court of South Africa, Case CCT 17/00 2000, decision of 29 September 2000.
http://www.saflii.org/za/cases/ZACC/2000/17.html.
(accessed Sept 21, 2008).
67
Eldridge v British Columbia, [1997] 3 S.C.R. 624.
http://csc.lexum.umontreal.ca/en/1997/1997rcs3-624/1997rcs3-624.html.
(accessed Sept 21, 2008).
68
UNFPA. Culture
matters—working with communities and faith-based organisations: case studies
from country programs. New York: UNFPA, 2004.
69
HuntP. Report of the
Special Rapporteur on the right to the highest attainable standard of health to
the Commission on Human Rights, UN Doc E/CN.4/2005/51/Add.3. Geneva: United
Nations, 2005.
70
AkunyiliD. The fight against counterfeit drugs in Nigeria. In: Transparency
International—global corruption report 2006: corruption and health. Berlin: Transparency
International, 2006: 96-100.
71
GreenA. An
introduction to health planning for developing health systems. Oxford: OUP, 2007.
72
HuntPStewartRMesquitaJOldringL. Neglected
diseases: a human rights analysis. Geneva: Special Programme for Research and Training in
Tropical Diseases (TDR), 2007.
73
AlloteyPReidpathDGhalibHPagnoniFSkellyI. Efficacious, effective, and embedded interventions:
implementation research in infectious disease control. BMC Public Health 2008; 8: 343. CrossRef | PubMed
74
In: Chapman A, Russell S, eds. Core
obligations: building a framework for economic, social and cultural rights. Antwerp: Intersentia,
2002.
75
HuntPMacNaughtonG. Impact assessments, poverty and human rights: a case
study using the right to the highest attainable standard of health. http://www2.essex.ac.uk/human_rights_centre/rth/projects.shtm.
(accessed Aug 15, 2008).
76
Minister of Health v Treatment Action
Campaign. Constitutional Court of South Africa, Case CCT 8/02,
decision of 5 July 2002. http://www.saflii.org.za/za/cases/ZACC/2002/16.html.
(accessed Sept 21, 2008).
77
Paschim Banga Khet Mazdoor Samity v State of West
Bengal, 1996 SCJ 25: 29. http://www.commonlii.org//cgi-bin/disp.pl/in/cases/INSC/1996/659.html?query=paschim.
(accessed Sept 21, 2008).
78
WHO. Report
of the global partners' meeting on neglected tropical diseases: a turning point. Geneva: World Health
Organization, 2007.
79
UNAIDS. Enhancing
results by applying the Paris Declaration at sector level: progress update and
lessons learnt from aid effectiveness in AIDS responses. Geneva: UNAIDS, 2008.
80
WHO. Framework Convention on Tobacco Control, adopted by the
56th World Health Assembly. http://www.who.int/fctc/en/.
(accessed Sept 21, 2008).
81
SkoglyS. Beyond
national borders: States' human rights obligations in international cooperation. London: Intersentia, 2006.
82
High Level Forum on Aid Effectiveness. Paris
declaration on aid effectiveness. http://www.oecd.org/document/18/0,3343,en_2649_3236398_35401554_1_1_1_1,00.html.
(accessed Sept 21, 2008).
83
International Council on Human Rights Policy.
Duties sans frontiers: human rights and global
social justice. Versoix: International Council on Human Rights Policy, 2003.
84
Straight Talk Foundation. http://www.straight-talk.or.ug/.
(accessed Oct 14, 2008).
85
HuntP. Report of the
UN Special Rapporteur on the right to the highest attainable standard of health
to the Human Rights Council, UN Doc A/HRC/7/11/Add.2. Geneva: United
Nations, 2008.
86
DarrowM. Between light
and shadow: the World Bank, the International Monetary Fund and international
human rights law. Portland: Hart, 2003.
87
In: Van Genugten W, Hunt P, Matthews S, eds. World Bank, IMF and human rights. Nijmegen: Wolf, 2003.
88
PottsH. Accountability
and the right to the highest attainable standard of health. Colchester: Human
Rights Centre, University of Essex, 2008.
89
ClaphamA. Human rights
obligations of non-state actors. Oxford: Oxford University Press, 2006.
90
New Vision. Health rights unit launched. Kampala: New Vision, Oct 1, 2008.
91
NolteEMcKeeMWaitS. Describing and evaluating health systems. In: Bowling A, Ebrahim S, eds. Handbook of
health research methods. New York: Open University Press, 2006: 12-43.
92
NeumanE. Do international human rights treaties improve respect
for human rights?. J Conflict Resolut 2005; 49: 6. PubMed
93
NolteEMcKeeM. Measuring the health of nations: analysis of mortality
amenable to health care. BMJ 2003; 327: 1129-1132. PubMed
94
International conference on primary health
care. Declaration of Alma-Ata. Alma-Ata, USSR: World
Health Organization, 1978.
95
Committee on the Rights of the Child. HIV/AIDS and the rights of the child.
March 17, 2003. CRC/GC/2003/3, General Comment 3.
96
Committee on the Rights of the Child. Adolescent health and development in the
context of the Convention on the Rights of the Child. July 1, 2003.
CRC/GC/2003/4, General Comment 4.
97
Committee on the Elimination of Discrimination against Women. Women and health.
A/54/38/Rev.1, chapter 1, General Recommendation 24.
98
HuntP. Report of the
Special Rapporteur on the right to the highest attainable standard of health to
the Commissioner on Human Rights, UN Doc E/CN.4/2006/48. Geneva: United
Nations, 2006.
99
UNDP.
Human development reports. http://hdr.undp.org/en/statistics/.
(accessed Aug 15, 2008).
100
UN. Report on indicators for promoting and monitoring the
implementation of human rights. HRI/MC/2008/3. http://www2.ohchr.org/english/bodies/icm-mc/documents.htm.
(accessed Dec 1, 2008).
101
UN. United Nations Millennium Development Goals Indicators.
http://mdgs.un.org/unsd/mdg/Default.aspx. (accessed Aug 15, 2008).
102
UN Office of the High Commissioner for Human
Rights. Geneva. Principles and guidelines
for a human rights approach to poverty reduction strategies. Geneva: UN, 2007.
103
WHO. Medicines
strategy 2004—2007. Geneva: World Health Organisation, 2004.
104
UNICEF. Monitoring
and statistics: core indicators in depth. http://www.unicef.org/statistics/index_24296.html.
(accessed Aug 15, 2008).
105
UNAIDS. 2006
Report on the global epidemic. Geneva: UNAIDS, 2006.
106
The World Bank. World
Development Indicators 2007. http://web.worldbank.org/WBSITE/EXTERNAL/DATASTATISTICS/0,,contentMDK:21298138∼pagePK:64133150∼piPK:64133175∼theSitePK:239419,00.html.
(accessed Aug 15, 2008).
107
The World Bank. Governance
Matters VI: aggregate and individual governance indicators 1996—2006. http://www-wds.worldbank.org/external/default/WDSContentServer/WDSP/IB/2007/07/10/000016406_20070710125923/Rendered/PDF/wps4280.pdf.
(accessed Aug 15, 2008).
108
WHO. Indigenous
peoples' health. WHO/SDE/HSD/99. Geneva: World Health Organization, 2006.
109
CRR. Broken
promises, human rights, accountability, and maternal death in Nigeria. Centre for
Reproductive Rights, 2008.
110
PHR. Deadly
delays: maternal mortality in Peru—a rights-based approach to safe motherhood. Physicians for Human
Rights, 2008.
111
HuntPMesquitaJ. Reducing
maternal mortality: the contribution of the right to the highest attainable
standard of health. University of Essex, 2006.
112
UNDP. Beyond
scarcity: power, poverty and the global water crisis. New York: Palgrave
Macmillan, 2006.
113
United States National Library of Medicine
National Institutes of Health. International Committee of Medical Journal Editors
Uniform Requirements for Manuscripts Submitted to Biomedical Journals: sample
references. http://www.nlm.nih.gov/bsd/uniform_requirements.html.
(accessed Sept 21, 2008).
114
OECD.
Ratification of the Convention on the OECD.
http://www.oecd.org/document/58/0,3343,en_2649_34483_1889402_1_1_1_1,00.html.
(accessed Sept 21, 2008).
115
The World Bank. Cumulative
IDA Subscriptions and Contributions. http://siteresources.worldbank.org/IDA/Resources/CUMIDA2008.pdf.
(accessed May 20, 2008).
116
European Parliament and Council. Directive
95/46/EC of the European Parliament and of the Council. http://www.cdt.org/privacy/eudirective/EU_Directive_.html#HD_NM_10.
(accessed Aug 08, 2008).
117
HuntPMacNaughtonG. A human rights-based approach to health indicators.
In: Baderin M, Mccorquodale R, eds. Economic, social
and cultural rights in action. Oxford: Oxford University Press, 2007: 303-330.
118
WHO. Countries. http://www.who.int/countries/en/.
(accessed Sept 09, 2008).
119
WHOUNICEF. Global water assessment and sanitation report 2000.
http://www.wssinfo.org/pdf/GWSSA_2000_report.pdf.
(accessed May 23, 2008).
120
HowardGBartramJ. Domestic water quantity, service level and health.
http://www.who.int/water_sanitation_health/diseases/en/WSH0302.pdf.
(accessed Dec 20, 2007).
121
WHOUNICEF. Joint monitoring programme for water supply and
sanitation, 2008. http://www.wssinfo.org/en/welcome.html.
(accessed Aug 8, 2008).
122
National Institute of Statistics. Annual report
of National Institute of Statistics, chapter Housing and Public Utilities.
http://www.insse.ro/cms/files/pdf/ro/cap5.pdf. (accessed July 23, 2008).
123
WHO. WHO
Multi-country study on women's health and domestic violence against women. Geneva: World Health
Organization, 2005.
124
WHO. World Health survey results. http://www.who.int/healthinfo/survey/en/. (accessed July 23, 2008).
125
The World Bank. Data and
statistics 2008. http://go.worldbank.org/D7SN0B8YU0.
(accessed Sept 21, 2008).
126
WHO, UNICEF, UNFPA, and the World Bank.
Maternal mortality in 2005. Geneva: World Health
Organization, 2007.
127
UN-OHCHR. Fact sheet no 19 national institutions for the
promotion and protection of human rights. Geneva: United Nations, 1993.
128
GAVI.
Health system strengthening. http://www.gavialliance.org/vision/policies/hss/index.php.
(accessed Sept 21, 2008).
129
Högskoleförordning. SFS 1993: 100
Amendment SFS 2007: 638. http://www.notisum.se/index2.aspsTemplate=/template/index.asp&iMenuID=314&iMiddleID=285&iParentMenuID=236&iLanguageID=1.
(accessed Sept 21, 2008).
130
Department of Health. Human rights
in healthcare evaluation. http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/DH_088979.
(accessed Nov 30, 2008).
131
WHO. Country Health information systems. http://www.who.int/healthinfo/systems/en/. (accessed Aug 8, 2008).
132
WHO. Department of Economic and Social Affairs' principles
and recommendations for a vital statistics system revision. http://unstats.un.org/unsd/publication/SeriesM/SeriesM_19rev2E.pdf.
(accessed June 15, 2008).
133
WHO. Beyond
the numbers: reviewing maternal deaths and complications to make pregnancy
safer. Geneva:
World Health Organization, 2004.
134
WHO. International statistical classification of diseases
and related health problems 10th revision version for 2007. http://www.who.int/classifications/apps/icd/icd10online/.
(accessed Sept 21, 2008).
135
Robertson D, Bedell R, Lavery J, Upshur R. What kind of evidence do we need to
justify humanitarian medical aid? Lancet360: 330—33.
136
WHO. Commission
on social determinants of health—final report. Geneva: World Health Organization, 2008.
137
United Nations General Assembly Special
Session on HIV/AIDS. Guidelines on construction of core indicators in
relation to monitoring the declaration of commitment on HIV/AIDS. http://www.measuredhs.com/hivdata/guides/ungassmeguidejuly2005.pdf.
(accessed Aug 8, 2008).
138
WHO. World
Health Report 2005: Make every mother and child count. Geneva: World Health
Organization, 2005.
139
WHO, UNICEF. WHO
vaccine-preventable diseases monitoring system. http://whqlibdoc.who.int/hq/2007/who_IVB_2007_eng.pdf.
(accessed May 20, 2008).
140
Demographic and Health Surveys. Model “A”
questionnaire with commentary for high contraceptive prevalence countries.
http://www.measuredhs.com/pubs/pdf/DHSQ4/DHS-IV-Model-A.pdf.pdf.
(accessed Sept 15, 2008).
141
WHO. Summary
report: WHO multi-country study on women's health and domestic violence against
women. Geneva:
World Health Organization, 2005.
142
Abuja Declaration. AIDS is a
state of emergency in the continent. Adopted 24—27 April 2001. http://www.un.org/ga/aids/pdf/abuja_declaration.pdf. (accessed Sept 21, 2008).
143
UNDP.
MDG Series metadata. http://millenniumindicators.un.org/unsd/mdg/Metadata.aspx?IndicatorId=0&SeriesId=776.
(accessed Sept 21, 2008).
144
International Covenant on Civil and Political
Rights (ICCPR). New York, United Nations, 1966. United Nations G.A.
Res. 2200A (XXI). UN GAOR, 21st Session, Supp. No. 16, at 52, UN Doc. A/6316,
entered into force 23 March 1976. http://www.unhchr.ch/html/menu3/b/a_ccpr.htm.
(accessed Sept 21, 2008).
145
UN Human Rights Council Res 5/1.
Institution-building of the United Nations Human Rights Council. http://www2.ohchr.org/english/bodies/hrcouncil/. (accessed Sept 21, 2008).
146
OHCHR. Economic,
social and cultural rights: handbook for national human rights institutions. Geneva: OHCHR, 2005.
147
Human Rights and Equal Opportunity Commission.
Social justice report 2005. Canberra: Human
Rights Equality Commission, 2005.
148
DuBoisM. Civilian protection and humanitarian advocacy:
strategies and (false?) dilemmas. Humanitarian
Exch 2008; 39: 12-15. PubMed
149
HuntP. Report of the
UN Special Rapporteur on the right to the highest attainable standard of health
to the United Nations General Assembly UN Doc A/63/263, 2008. New York: United
Nations, 2008.
a Nordic School
of Public Health, Gothenburg, Sweden
b Human Rights
Centre, University of Essex, Colchester, UK
c School of
Health and Human Sciences, University of Essex, Colchester, UK
d Office of the
Mayor of Bogata, Colombia
e Foundation for
Alterative Social Development, Cuenca, Ecuador
f Health Team
National Coordinator, CARE Peru, Lima, Peru
g National
Health Council Secretariat, Ministry of Health, Lima, Peru
h WHO-Western
Pacific Regional Office, Manila, Philippines
i Centre of
Health Policies and Services, Bucharest, Romania
j Department of
Public Health, Victor Babes University of Medicine and Pharmacy, Timisoara,
Romania
================================================================
To contact the list administrator, or to leave the list, send an email to:
wunrn_listserve-request@lists.wunrn.com. Thank you.




